The influence of radiological tumor growth pattern on sino‑nasal health in pituitary adenomas
- Authors:
- Published online on: January 26, 2024 https://doi.org/10.3892/ol.2024.14258
- Article Number: 125
-
Copyright: © Walbrodt et al. This is an open access article distributed under the terms of Creative Commons Attribution License.
Abstract
Introduction
Pituitary adenomas account for one of the most common mass lesions of the brain with an estimated prevalence of 20% in the population and one third who become clinically apparent (1). Due to their localization deep in the skull base, endoscopically or microscopically resection via the minimally invasive endonasal, transsphenoidal approach is the gold standard wherever it is feasible.
In recent years, research on sino-nasal health (SNH) following endonasal surgery experienced more attention, because at least temporarily sino-nasal complaints are among the most common morbidities after surgery (2,3). Both surgical techniques have been compared regarding their influence on SNH before and after surgery, while the influence of radiological tumor growth pattern on SNH has not been addressed yet.
Radiologic classification of pituitary gland tumors started in the 1970s with the Hardy scale, which describes the degree of sellar destruction (grade) and extrasellar growth (stage) based on CT scans and encephalography (4). Although the Hardy classification was developed in the pre-MRI era, it is still used nowadays and has a good reliability of the scale's upper and lower end where parasellar tumor growth is obvious, though the interrater reliability of its intermediate scores has come under scrutiny (5). The Knosp classification is the most popular scale today. It was introduced 1993 and is based on coronal magnetic resonance images of the Sella region describing the invasion of the cavernous sinus space using the intra- and supracavernous internal carotid arteries as a landmark (6). Due to its simplicity and acceptable interrater reliability, it has a good clinical validity and predictive value for gross total reduction (7).
Both classifications have already been evaluated in terms of their predictive value in surgical cure while their predictive value on SNH after surgery remains unknown. Hence, our novel study aimed to compare patients with radiologically low and high invasive lesions and the pre- and postoperative outcome after endoscopic endonasal pituitary adenoma surgery regarding the patients' experienced SNH.
Materials and methods
Sino-Nasal Outcome Test for Neurosurgery (SNOT-NC) questionnaire
The SNOT-NC is a self-report questionnaire that has been validated for pituitary adenoma surgery. It is partially based on the German version of the Sino-Nasal Outcome Test (SNOT-22 questionnaire) (8,9) and was developed to assess the clinical outcome of patients undergoing transnasal endoscopic skull base surgery (10). The test comprises 23 items in five domains to detect the degree of impairment for each domain. Domains evaluate nasal discomfort, sleep problems/reduced productivity, ear and head discomfort, visual impairment and a total score featuring the listed four domains and additional olfactory disturbance related items. The more points scored per item, the higher the total score and the associated impairment. Patients were asked to fill in the SNOT-NC questionnaire the day before surgery and at Follow-up (FU).
Radiological classifications
Tumor size and local invasion were classified using dichotomized versions of Hardy's classification (Table I) of pituitary tumors and the Knosp classification (Table II) of cavernous sinus invasion of pituitary macroadenomas on preoperatively obtained contrast enhanced T1 weighted magnetic resonance imaging (MRI) data. Wherever available, preoperative CT scans were additionally used to assess sphenoid bone invasion.
Statistical analysis
Statistical analyses were conducted with SPSS version 29, IBM Inc. Depending on their Knosp score being ≥3 and <3, patients were dichotomized between low and high invasive lesions. In addition, Hardy classification has been subdivided into two domains: the degree of sellar floor destruction and the extent of supra- and parasellar tumor growth. Sellar floor destruction condenses the grades 0, 1 and 2 to lowly invasive; the grades 3 and 4 are condensed to highly invasive. Grades A and B of Hardy's degree of extrasellar growth were considered lowly invasive; the grades C, D and E constituted the highly invasive group. Dichotomization of both scales in small and large lesions was inevitable to achieve a reliable number of cases. Delta values have been calculated from pre- and post-surgery SNOT-NC results (delta score=pre-operative score-post-operative score) and unpaired t-tests were used to assess significant differences between the groups of lowly and highly invasive tumors for each domain of the SNOT-NC questionnaire. Paired t-tests were used for all SNOT-NC components to examine the effect of surgery within those groups. Levene's test was used for every t-test to control for equal variance. Effect sizes were estimated using Cohen's d (small <0.2, medium ≤0.5 and large effect >0.5) for all t-tests. Both groups with lowly and highly invasive lesions were compared regarding postoperative complications and possible covariates by using the χ2 test. If the sample size did not meet the χ2 test criteria, Fisher's exact test was used. For the covariate age we used the Mann-Whitney-U test. P<0.05 was considered to indicate a statistically significant difference.
Data acquisition
Patient data was collected prospectively between August 1st, 2016 and August 31st, 2022 at the Department of Neurosurgery and Spine Surgery at the University Hospital Essen. All patients underwent pituitary tumor surgery via the endoscopic, transsphenoidal bi-nostril approach. Follow-up (FU) examinations were conducted 3–6 months after surgery. The study was conducted in accordance with the 1964 Declaration of Helsinki and was approved by the institutional review board of the Medical Faculty of the University Hospital Essen (identification number: 14-5791-BO). Written informed consent was obtained from all individual participants included in the study.
Results
General characteristics
A total of 101 patients who underwent endoscopic pituitary adenoma surgery with completed pre- and postoperative SNOT-NC questionnaires were included in this study. Inclusion criteria were age over 18 and histologically confirmed pituitary adenoma; individuals with incomplete Knosp and/or Hardy Scores, incomplete questionnaires for SNOT-NC and non-adenoma histology were excluded. 46 (45.5%) of the total cohort were females and the mean age was 54.7 (SEM ±1.32). All patients had Doyle splints inserted for approx. ten days postoperatively. All surgeries have been performed by five well experienced surgeons.
Postoperative complications and covariates
Postoperative complications comprised electrolyte disbalances due to the syndrome of inappropriate antidiuretic hormone secretion and diabetes insipidus as well as lumbar drainage, meningitis and rhinoliquorrhea (Table III). Although postoperative hormonal disturbances were more frequent in patients with Knosp 3–4, considering the group size this effect was not statistically significant for Knosp and both Hardy domains (all P≥0.081). However, postoperative lumbar drainage was significantly more often necessary in highly invasive tumors for all scales (all P≤0.044). Meningitis and rhinoliquorrhea occurred seldomly and independently from the tumor invasiveness. Postoperative epistaxis with the need for surgical intervention did not occur in our sample size.
Table III.Postoperative complications for lowly and highly invasive Knosp and Hardy classified tumors. |
In addition, we tried to identify possible SNH influencing covariates such as age, hormonal activity and syndromes such as Cushing's disease and Acromegalia (Table IV). In general, we did not find significant differences for most covariates. However, individuals with Knosp 0-II tumors were significantly younger than those with Knosp III–IV lesions. In addition, the gender distribution was significantly uneven between both groups for Hardy infrasellar lesions.
Table IV.Covariates for lowly and highly invasive Knosp and Hardy classified tumors. Chi-squared tests were used wherever no other test method is given. |
Knosp classification
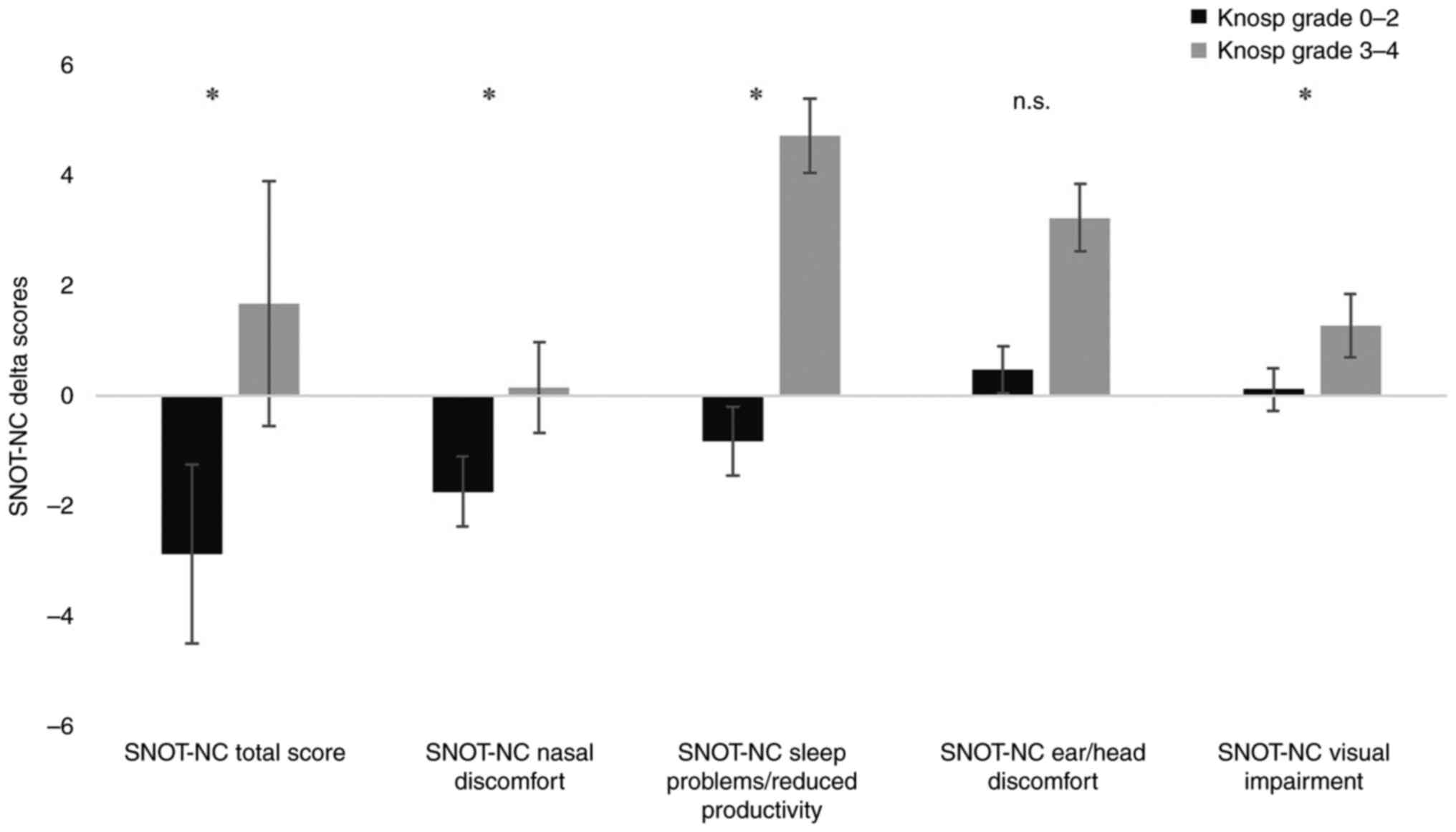
The SNOT-NC questionnaire revealed statistically significant differences between the two Knosp subgroups SNOT-NC's total score (P=0.048, d=0.3), nasal discomfort (P=0.034, d=0.37), sleep problems (P=0.024, d=0.4) and visual impairment (P=0.042, d=0.35) as depicted in Fig. 1.
Assessing the effects of surgery within the group of Knosp lowly invasive tumors (n=57), we saw a significant worsening for the SNOT-NC total score (P=0.04, d=0.2) and nasal discomfort (P=0.004, d=0.37). In contrast, sleep problems, ear/head discomfort and visual impairment did not change significantly after surgery. However, there was a tendency for increased sleep problems as postoperative score rose by 0.8 points on average (P=0.096).
For Knosp high graded tumors (n=44), patients reported a significant improvement after surgery for SNOT-NC visual impairment (P=0.016, d=0.33). Moreover, we saw a tendency for reduced sleep problems (P=0.067, d=0.23) postoperatively, while all other SNOT-NC domains did not appear to be affected by surgery (see Table V).
Table V.Scores before and after surgery for both Knosp groups, paired t-tests show significant differences. |
Hardy classification
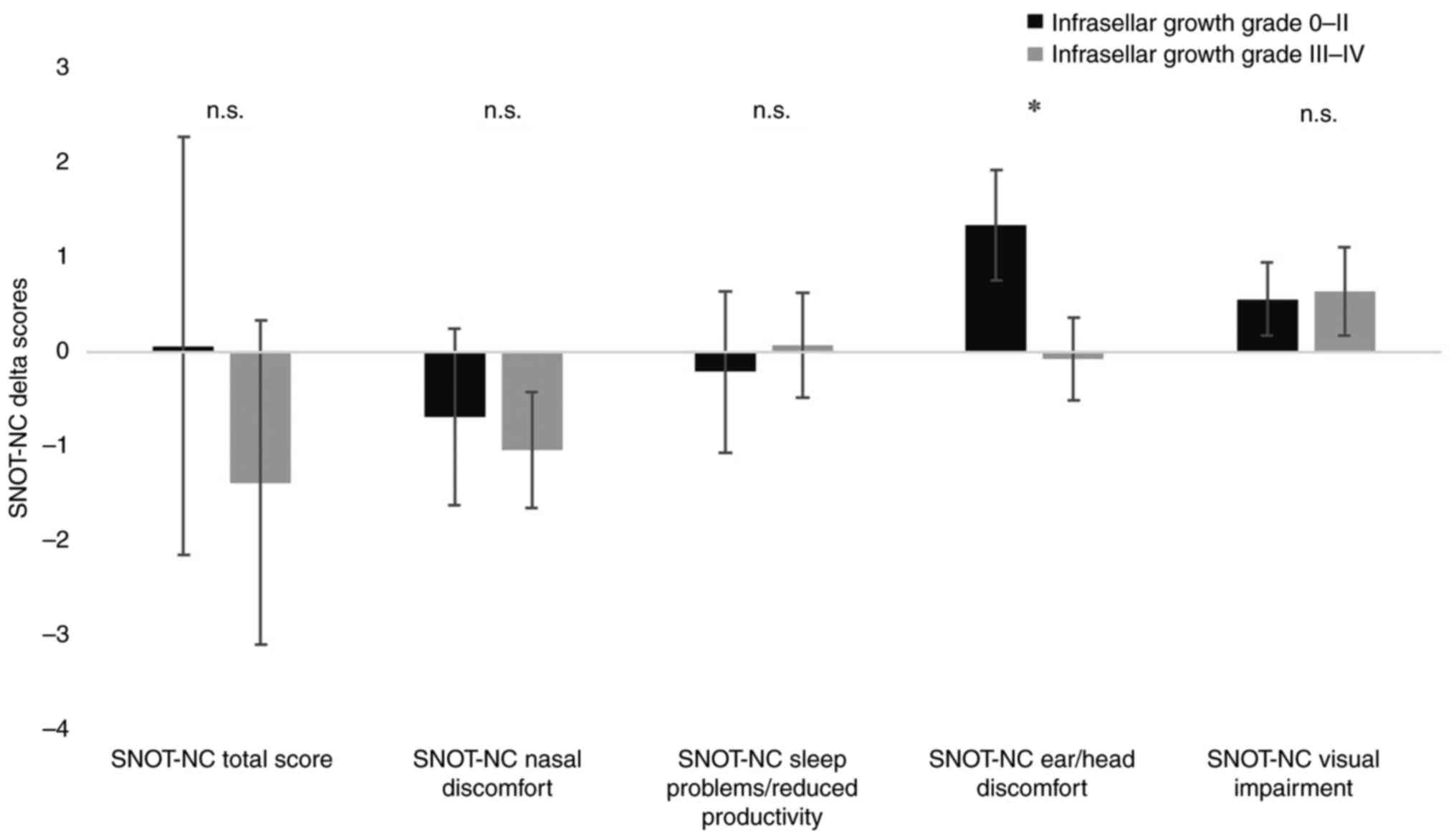
Assessing the suprasellar domain of the Hardy classification, unpaired t-tests yielded no significant differences between the low invasive group (Hardy suprasellar growth grades A-B) and the high invasive group (grades C-E) independently of the SNOT-NC domains. However, assessing Hardy's sellar erosion domain, a decreased ear/head discomfort for lowly invasive lesions compared to patients grades III–IV could be detected (P=0.03, d=0.4) (Fig. 2). In addition, patients with III–IV lesions had higher SNOT-NC total scores on average than patients with 0-II lesions. However, this effect did not prove to be significant due to the high standard deviation of both subgroups (P=0.3)
While Hardy's suprasellar domain did not show significant differences between lowly and highly invasive tumor growth, patients with lesions of low graded suprasellar growth (n=79) exhibited a rise of 1.3 points for SNOT-NC's nasal discomfort domain after surgery (P=0.013, d=0.26). All other SNOT-NC domains did not show relevant effects of surgery at FU. The 22 patients with high graded suprasellar growth (C-E) showed a trend towards reduced visual impairment, though the t-test remained not significant (P=0.058, d=0.35) (Table VI).
Table VI.SNOT-NC scores before and after surgery for both Hardy's suprasellar growth groups, paired t-tests evaluate significant differences. |
Assessing the group of lowly invasive sellar eroding lesions (n=34) we observed a significant decrease of ear/head discomfort after surgery (P=0.014, d=0.4). This effect could not be seen in patients with infrasellar erosion grades III–IV, who already had lower baseline levels (9.03 vs. 10.52) and lower levels at FU (9.11 vs. 9.18) on average. However, patients with III–IV graded lesions revealed a significant deterioration of SNOT-NC's nasal discomfort domain (P=0.046, d=0.2) at FU, while both groups of lowly and highly invasive sellar eroding lesions showed minor tendencies for decreased visual impairment at FU (P=0.082, P=0.085, respectively) (Table VII).
Table VII.SNOT-NC scores before and after surgery for both Hardy's infrasellar growth groups, paired t-tests evaluate significant differences. |
Discussion
In this study, our objective was to identify the influence of presurgical radiological tumor size on SNH suggesting that patients with smaller lesions experience fewer symptoms due to lower tumor invasiveness and lesser scope of surgery. While large, invasive pituitary tumor growth has been shown to be a predictor for increased complications and incomplete resection in endoscopic transsphenoidal surgery (11), the influence of tumor morphology on SNH has not been evaluated yet. In addition, the effect of endoscopic transsphenoidal surgery on SNH and quality of life has been examined with diverging results (12–14).
Our results showed that the SNOT-NC questionnaire shows significant differences between Knosp 0-II and Knosp III–IV lesions for SNOT-NC's total, nasal discomfort, sleep problems/reduced productivity and visual impairment after surgery. Moreover, patients with high graded Knosp lesions had better scores on average for every SNOT-NC domain than the low graded cohort at the time of FU, while those with low graded lesions seem to experience a deterioration in three of five domains after surgery. Considering the average values before surgery, individuals with Knosp III–IV tumors had higher scores than individuals with Knosp 0-II tumors except for ear/head discomfort. After surgery, patients with highly invasive tumors had better average scores for every SNOT-NC domain compared to the post-operative scores of the lowly invasive tumors. For ear/head discomfort and visual impairment the FU scores were even below the baseline scores of patients with lowly invasive tumors. However, assessing the effects of surgery for both groups-Knosp 0-II and III–IV-we only found a significant decrease of SNH for SNOT-NC's nasal discomfort and total score domain for Knosp 0-II tumors and according to Cohen's d, these effects were mild to moderate.
These findings outline that patients experience SNH differently as assessed by self-reporting questionnaires. Higher rates of deterioration of SNH in patients with Knosp low graded tumors appeared to be driven by the patient's perception and expectations from surgery. Those patients were less affected by tumor growth before surgery and had therefore lower (better) test results preoperatively. After surgery, they seemed to be focused on postoperative sequelae. Patients with Knosp III–IV tumors report better SNOT-NC scores at the time of FU, because they likely had more severe symptoms before surgery, which improved after surgery. E.g. sleep disturbance in patients with pituitary tumors has been described before and appears to be a consequence of direct and indirect effects of hormonal overproduction with circadian rhythm abnormalities due to compression of the optic chiasm (15) and/or acromegaly-related sleep apnea syndrome. These symptoms might be more under control due to hormonal excess after surgery being reduced. However, alleviation of sleep disturbances after tumor surgery has been discussed controversially (16–18) and though we could see an improvement after surgery in the Knosp classification, Hardy's extrasellar growth classification did not yield significant differences.
Although Hardy's suprasellar growth classification describes the compression of the optic chiasm better than Knosp, we did not observe significant differences between the grades A-B and C-E regarding SNH. Moreover, a relevant effect of surgery could only be seen in SNOT-NC's nasal discomfort domain for the lowly invasive grades A-B, which increased at FU. Other SNOT-NC domains showed similar baseline and FU scores for lowly invasive tumors. In addition, Individuals with C-E graded lesions reported slightly better scores at the time of FU. Still, no statistical significance was found except for a weak trend regarding reduced visual impairment. However, the sample size was small in this group with 22 individuals, which weakens the statistical power.
Regarding Hardy's infrasellar growth classification, patients with 0-II lesions showed a minor improvement for SNOT-NC's visual impairment score, but also a significant decrease in ear/head discomfort compared to Hardy III–IV graded patients, whose scores at FU were close to baseline values. Furthermore, patients with Hardy III–IV lesions appeared to be more negatively affected by surgery due to significantly higher nasal discomfort at FU, although baseline levels did not differ much from those with 0-II graded tumors (13.27 vs. 13.24).
These findings implicate that large tumor growth through the sellar floor might be a risk factor for reduced SNH conceivably due to a greater scope of surgery which might be accompanied by greater destruction of the local mucosa. Moreover, negative effects of extended surgical intervention on SNH have already been reported for the Hadad septal flap (19). In addition, Hallén et al and Chmielewski et al reported that previous nasal surgery might be a risk factor for decreased SNH after endoscopic pituitary adenomectomy (20,21) underlining the role of unaffected mucosa for SNH.
Furthermore, neither postoperative complications nor most covariates did differ significantly between Hardy/Knosp low and high graded lesions. In fact, lumbar drainage was even more common in patients with high graded lesions, but SNH even improved at FU for those patients. These findings suggest SNH is not influenced by postoperative complications or covariates at the time of FU. However, the list of possible covariates in our study is incomplete and data regarding BMI and morphology of the sphenoid sinus is missing. Especially the influence of the morphology of the sphenoid sinus on SNH is poorly understood and should be addressed in further research.
While there are some studies who investigate health-related quality of life (HR-QoL) for pituitary adenoma surgery, there is still a lack of studies that specifically assess SNH. Considering HR-QoL several reports show that QoL is reduced before and after transsphenoidal surgery in patients with pituitary adenoma (22–24). However, a meta-analysis by Bhenswala et al, who examined SNH before and after endoscopic, endonasal skull base surgery and not exclusively targeting pituitary adenoma pathologies, describes a usually 4 week long deterioration of SNH, followed by a significant improvement, even beyond the patient's preoperative SNH, evaluated by the SNOT-22 test (25). In addition, Little et al report a temporary deterioration of SNH with complete recovery at 3 months after surgery (12). Based on our data, we suggest SNH is influenced by patients' expectations towards surgery and might not be completely recovered within the first 3–6 months after operation for patients who had few symptoms before treatment. Of course, it has to be pointed out that we used a different questionnaire. But as the SNOT-NC is derived from the SNOT-22, it should be allowed to assume an acceptable comparability. In conclusion, detailed information regarding SNH should be part of every preoperative explanatory meeting to avoid false expectations of those patients.
The study has several limitations that might affect the results. First, wherever possible preoperative MRI and additional CT scans have been consulted to classify the tumor growth pattern, but especially for the sellar floor erosion there is a risk of interrater bias (5). Additionally, no further assessments such as rhinoscopy have been conducted to objectify reported deteriorations or improvements of SNH and data about mental and physical health status has not been collected, what has been described in literature as part of the patient's burden with pituitary adenoma diagnosis. Although the SNOT-NC questionnaire is validated for transnasal endoscopic pituitary adenoma surgery, there has been little data published and normal values for healthy individuals are absent. This issue should be addressed in further studies to examine the patient's sino-nasal constraints compared to those of healthy individuals for a better prediction of the impact of treatment.
In conclusion, we found new evidence that SNH is subjective and might be dependent on radiological tumor growth patterns. Our data demonstrate that patients with less invasive tumors and fewer symptoms are more prone to experience a deterioration in SNH after the procedure than patients with severe symptoms. In addition, sellar floor erosion might be a factor prognosticating increased nasal discomfort after surgery.
Acknowledgements
The authors would like to acknowledge the contribution of Mrs. Janine Szybowicz (Department of Neurosurgery and Spine Surgery, University Hospital Essen) in the data acquisition and organization.
Funding
Funding: No funding was received.
Availability of data and materials
The datasets generated and/or analyzed during the current study are not publicly available due to the protected privacy data of the participating patients but may be requested from the corresponding author.
Authors' contributions
SW was involved in writing the manuscript, statistical analysis, designing the study protocol, interpreting the results, creating tables and figures, and patient recruitment and assessment. WXC performed statistical analysis and reviewed the manuscript. MS provided support in evaluating the radiological scores and reviewed the manuscript. CD provided support in evaluating the radiological scores. TFD, MC, HHG, RJ, MDO, AL, AKU, OG, IKA and BS were responsible for patient recruitment and assessment and reviewed the manuscript. KHW and US contributed to study conception, study design and reviewed the manuscript. YA designed the study protocol, interpreted the results, wrote and reviewed the manuscript. WXC and YA confirmed the authenticity of all the raw data. All authors read and approved the final manuscript.
Ethics approval and consent to participate
The present study was conducted in accordance with the 1964 Declaration of Helsinki and was approved by the institutional review board of the Medical Faculty of the University Hospital Essen (approval no. 14-5791-BO). Written informed consent was obtained from all individual participants included in the study.
Patient consent for publication
All participants included in this study gave written consent to the use of their data for the purpose of scientific research and publication.
Competing interests
The authors declare that they have no competing interests.
References
|
Asa SL and Ezzat S: The pathogenesis of pituitary tumours. Nat Rev Cancer. 2:8368492002. View Article : Google Scholar : PubMed/NCBI | |
|
Balaker AE, Bergsneider M, Martin NA and Wang MB: Evolution of sinonasal symptoms following endoscopic anterior skull base surgery. Skull Base. 20:245–251. 2010. View Article : Google Scholar : PubMed/NCBI | |
|
Pledger CL, Elzoghby MA, Oldfield EH, Payne SC and Jane JA: Prospective comparison of sinonasal outcomes after microscopic sublabial or endoscopic endonasal transsphenoidal surgery for nonfunctioning pituitary adenomas. J Neurosurg. 125:323–333. 2016. View Article : Google Scholar : PubMed/NCBI | |
|
Wilson CB: A decade of pituitary microsurgery. The Herbert Olivecrona lecture. J Neurosurg. 61:814–833. 1984. View Article : Google Scholar : PubMed/NCBI | |
|
Mooney M, Hardesty D, Sheehy J, Bird C, Chapple K, White W and Little AS: Rater reliability of the hardy classification for pituitary adenomas in the magnetic resonance imaging era. J Neurol Surg B Skull Base. 78:413–418. 2017. View Article : Google Scholar : PubMed/NCBI | |
|
Knosp E, Steiner E, Kitz K and Matula C: Pituitary adenomas with invasion of the cavernous sinus space. Neurosurgery. 33:610–618. 1993. View Article : Google Scholar : PubMed/NCBI | |
|
Lee SH, Park JS, Lee S, Kim SW and Hong YK: Parasellar extension grades and surgical extent in endoscopic endonasal transsphenoidal surgery for pituitary adenomas: A single surgeon's consecutive series with the aspects of reliability and clinical validity. J Korean Neurosurg Soc. 59:577–583. 2016. View Article : Google Scholar : PubMed/NCBI | |
|
Hopkins C, Gillett S, Slack R, Lund VJ and Browne JP: Psychometric validity of the 22-item Sinonasal Outcome Test. Clin Otolaryngol. 34:447–454. 2009. View Article : Google Scholar : PubMed/NCBI | |
|
Baumann I, Blumenstock G, DeMaddalena H, Piccirillo JF and Plinkert PK: Quality of life in patients with chronic rhinosinusitis: Validation of the Sino-Nasal Outcome Test-20 German Adapted Version. HNO. 55:42–47. 2007.(In German). View Article : Google Scholar : PubMed/NCBI | |
|
Ahmadipour Y, Müller O, Kreitschmann-Andermahr I, Mattheis S, Sure U and Hütter BO: Development, reliability, validity and sensitivity of the Sino-Nasal Outcome Test for Neurosurgery (SNOT-NC). Eur Arch Otorhinolaryngol. 277:235–244. 2020. View Article : Google Scholar : PubMed/NCBI | |
|
Heffernan AT, Han JK, Campbell J, Reese J, Day WG, Edwards J, Singh RV, Zhu W and Lam KK: Predictive value of pituitary tumor morphology on outcomes and complications in endoscopic transsphenoidal surgery. World J Otorhinolaryngol Head Neck Surg. 8:321–329. 2022. View Article : Google Scholar : PubMed/NCBI | |
|
Little AS, Kelly DF, Milligan J, Griffiths C, Prevedello DM, Carrau RL, Rosseau G, Barkhoudarian G, Jahnke H, Chaloner C, et al: Comparison of sinonasal quality of life and health status in patients undergoing microscopic and endoscopic transsphenoidal surgery for pituitary lesions: A prospective cohort study. J Neurosurg. 123:799–807. 2015. View Article : Google Scholar : PubMed/NCBI | |
|
Graham SM, Iseli TA, Karnell LH, Clinger JD, Hitchon PW and Greenlee JDW: Endoscopic approach for pituitary surgery improves rhinologic outcomes. Ann Otol Rhinol Laryngol. 118:630–635. 2009. View Article : Google Scholar : PubMed/NCBI | |
|
Hong SD, Nam DH, Seol HJ, Choi NY, Kim HY, Chung SK, Kim HY, Chung SK and Dhong HJ: Endoscopic binostril versus transnasal transseptal microscopic pituitary surgery: Sinonasal quality of life and olfactory function. Am J Rhinol Allergy. 29:221–225. 2015. View Article : Google Scholar : PubMed/NCBI | |
|
Shibata S and Moore RY: Neuropeptide Y and optic chiasm stimulation affect suprachiasmatic nucleus circadian function in vitro. Brain Res. 615:95–100. 1993. View Article : Google Scholar : PubMed/NCBI | |
|
Sagan KP, Andrysiak-Mamos E, Tyburski E, Sagan LM and Syrenicz A: Quality of life and sleep in patients with pituitary adenoma in relation to tumor type and compression of the optic chiasm. J Clin Med. 10:18792021. View Article : Google Scholar : PubMed/NCBI | |
|
Chemla D, Attal P, Maione L, Veyer AS, Mroue G, Baud D, Salenave S, Kamenicky P, Bobin S and Chanson P: Impact of successful treatment of acromegaly on overnight heart rate variability and sleep apnea. J Clin Endocrinol Metab. 99:2925–2931. 2014. View Article : Google Scholar : PubMed/NCBI | |
|
Wolters TLC, Roerink SHPP, Drenthen LCA, van Haren-Willems JHGM, Wagenmakers MAEM, Smit JWA, Hermus ARMM and Netea-Maier RT: The course of obstructive sleep apnea syndrome in patients with acromegaly during treatment. J Clin Endocrinol Metab. 105:290–304. 2020. View Article : Google Scholar : PubMed/NCBI | |
|
Rotenberg BW, Saunders S and Duggal N: Olfactory outcomes after endoscopic transsphenoidal pituitary surgery. Laryngoscope. 121:1611–1613. 2011. View Article : Google Scholar : PubMed/NCBI | |
|
Hallén T, Olsson DS, Farahmand D, Esposito D, Olofsson AC, Jakobsson S, Jakobsson Ung E, Sahlstrand-Johnson P, Johannsson G, Skoglund T and Bergquist H: Sinonasal symptoms and Self-Reported health before and after endoscopic pituitary surgery-A Prospective study. J Neurol Surg B Skull Base. 83 (Suppl 2):e160–e168. 2022. View Article : Google Scholar : PubMed/NCBI | |
|
Chmielewski WX, Walbrodt S, Rauschenbach L, Chihi M, Gembruch O, Darkwah Oppong M, Schroer S, Wrede KH, Dammann P, Jabbarli R, et al: Pre-Surgery patient health contributes to aggravated sino-nasal outcome and quality of life after pituitary adenomectomy. Medicina (Kaunas). 59:592023. | |
|
Tanemura E, Nagatani T, Aimi Y, Kishida Y, Takeuchi K and Wakabayashi T: Quality of life in nonfunctioning pituitary macroadenoma patients before and after surgical treatment. Acta Neurochir (Wien). 154:1895–1902. 2012. View Article : Google Scholar : PubMed/NCBI | |
|
Dekkers OM, van der Klaauw AA, Pereira AM, Biermasz NR, Honkoop PJ, Roelfsema F, Smit JW and Romijn JA: Quality of life is decreased after treatment for nonfunctioning pituitary macroadenoma. J Clin Endocrinol Metab. 91:3364–3369. 2006. View Article : Google Scholar : PubMed/NCBI | |
|
Johnson MD, Woodburn CJ and Vance ML: Quality of life in patients with a pituitary adenoma. Pituitary. 6:81–17. 2003. View Article : Google Scholar : PubMed/NCBI | |
|
Bhenswala PN, Schlosser RJ, Nguyen SA, Munawar S and Rowan NR: Sinonasal quality-of-life outcomes after endoscopic endonasal skull base surgery. Int Forum Allergy Rhinol. 9:1105–1118. 2019. View Article : Google Scholar : PubMed/NCBI |