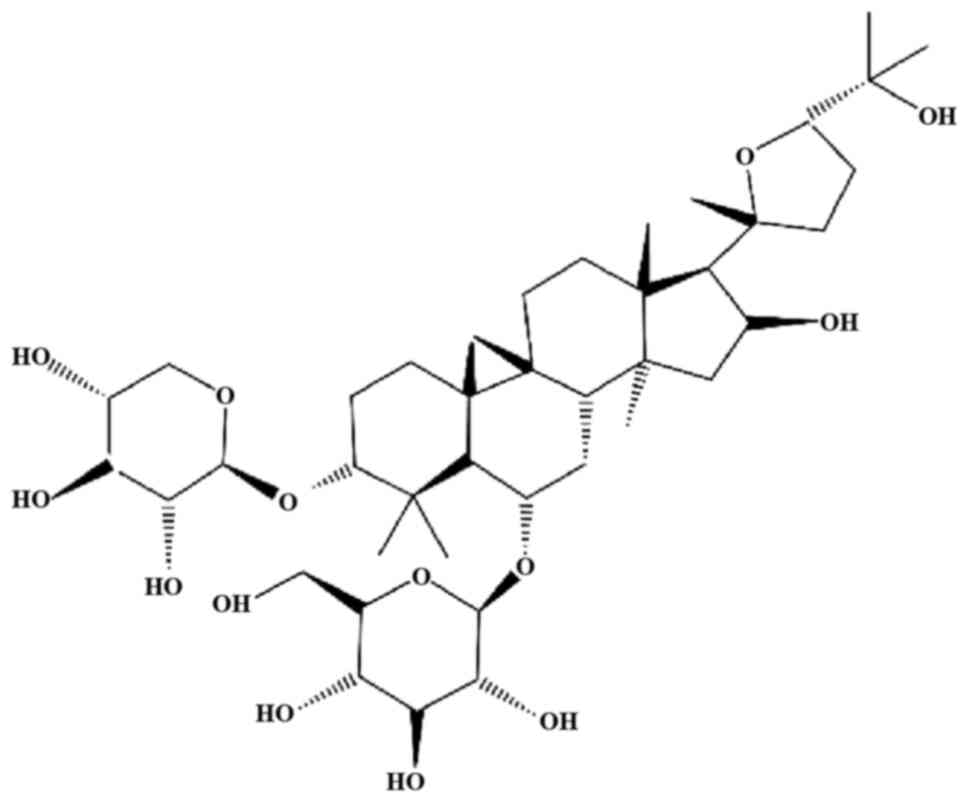
Molecular mechanisms of astragaloside‑IV in cancer therapy (Review)
- Authors:
- Tianqi Chen
- Peiying Yang
- Yingjie Jia
-
Affiliations: Department of Oncology, First Teaching Hospital of Tianjin University of Traditional Chinese Medicine, Tianjin 300380, P.R. China - Published online on: January 7, 2021 https://doi.org/10.3892/ijmm.2021.4846
- Article Number: 13
-
Copyright : © Chen et al. This is an open access article distributed under the terms of Creative Commons Attribution License [CC BY 4.0].
This article is mentioned in:
Abstract
 |
 |
 |
 |
|
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA and Jemal A: Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 68:394–424. 2018. View Article : Google Scholar : PubMed/NCBI | |
|
Chen J, Ni Y, Sun G, Zhu S, Zhao J, Wang Z, Zhang H, Zhu X, Zhang X, Dai J, et al: Survival outcomes of radical prostatectomy + extended pelvic lymph node dissection and radiotherapy in prostate cancer patients with a risk of lymph node invasion over 5%: A population-based analysis. Front Oncol. 10:6075762020. View Article : Google Scholar : PubMed/NCBI | |
|
Di Cintio F, Dal Bo M, Baboci L, De Mattia E, Polano M and Toffoli G: The molecular and microenvironmental landscape of glioblastomas: Implications for the novel treatment choices. Front Neurosci. 14:6036472020. View Article : Google Scholar : PubMed/NCBI | |
|
Li Y, Wang J, Ma X, Tan L, Yan Y, Xue C, Hui B, Liu R, Ma H and Ren J: A review of neoadjuvant chemoradiotherapy for locally advanced rectal cancer. Int J Biol Sci. 12:1022–1031. 2016. View Article : Google Scholar : PubMed/NCBI | |
|
Bhoday J, Glimelius B, Tait D, Glynne-Jones R, Adams R and Brown G: Session 4: What should we do for poor responders after chemoradiotherapy: Bad biology or should the fight go on? Colorectal Dis. 20(Suppl 1): 97–99. 2018. View Article : Google Scholar : PubMed/NCBI | |
|
Qi F, Zhao L, Zhou A, Zhang B, Li A, Wang Z and Han J: The advantages of using traditional Chinese medicine as an adjunctive therapy in the whole course of cancer treatment instead of only terminal stage of cancer. Biosci Trends. 9:16–34. 2015. View Article : Google Scholar : PubMed/NCBI | |
|
Jung Y, Jerng U and Lee S: A systematic review of anticancer effects of radix astragali. Chin J Integr Med. 22:225–236. 2016. View Article : Google Scholar | |
|
Li X, Qu L, Dong Y, Han L, Liu E, Fang S, Zhang Y and Wang T: A review of recent research progress on the astragalus genus. Molecules. 19:18850–18880. 2014. View Article : Google Scholar : PubMed/NCBI | |
|
Yu SY, Ouyang HT, Yang JY, Huang XL, Yang T, Duan JP, Cheng JP, Chen YX, Yang YJ and Qiong P: Subchronic toxicity studies of Radix Astragali extract in rats and dogs. J Ethnopharmacol. 110:352–355. 2007. View Article : Google Scholar | |
|
Gui D, Guo Y, Wang F, Liu W, Chen J, Chen Y, Huang J and Wang N: Astragaloside IV, a novel antioxidant, prevents glucose-induced podocyte apoptosis in vitro and in vivo. PLoS One. 7:e398242012. View Article : Google Scholar : PubMed/NCBI | |
|
Ren S, Zhang H, Mu Y, Sun M and Liu P: Pharmacological effects of Astragaloside IV: A literature review. J Tradit Chin Med. 33:413–416. 2013. View Article : Google Scholar : PubMed/NCBI | |
|
Zhao J, Yang P, Li F, Tao L, Ding H, Rui Y, Cao Z and Zhang W: Therapeutic effects of astragaloside IV on myocardial injuries: Multi-target identification and network analysis. PLoS One. 7:e449382012. View Article : Google Scholar : PubMed/NCBI | |
|
Xu W, Shao X, Tian L, Gu L, Zhang M, Wang Q, Wu B, Wang L, Yao J, Xu X, et al: Astragaloside IV ameliorates renal fibrosis via the inhibition of mitogen-activated protein kinases and antiapoptosis in vivo and in vitro. J Pharmacol Exp Ther. 350:552–562. 2014. View Article : Google Scholar : PubMed/NCBI | |
|
Karmakar S, Banik NL, Patel SJ and Ray SK: Curcumin activated both receptor-mediated and mitochondria-mediated proteolytic pathways for apoptosis in human glioblastoma T98G cells. Neurosci Lett. 407:53–58. 2006. View Article : Google Scholar : PubMed/NCBI | |
|
Bagci EZ, Vodovotz Y, Billiar TR, Ermentrout GB and Bahar I: Bistability in apoptosis: Roles of bax, bcl-2, and mitochondrial permeability transition pores. Biophys J. 90:1546–1559. 2006. View Article : Google Scholar | |
|
Sun P, Liu Y, Wang Q and Zhang B: Astragaloside IV inhibits human colorectal cancer cell growth. Front Biosci (Landmark Ed). 24:597–606. 2019. View Article : Google Scholar | |
|
Zheng Y, Dai Y, Liu W, Wang N, Cai Y, Wang S, Zhang F, Liu P, Chen Q and Wang Z: Astragaloside IV enhances taxol chemosensitivity of breast cancer via caveolin-1-targeting oxidant damage. J Cell Physiol. 234:4277–4290. 2019. View Article : Google Scholar | |
|
Jia L, Lv D, Zhang S, Wang Z and Zhou B: Astragaloside IV Inhibits the progression of non-small cell lung cancer through the Akt/GSK-3β/β-Catenin Pathway. Oncol Res. 27:503–508. 2019. View Article : Google Scholar | |
|
Zhao Y, Wang L, Wang Y, Dong S, Yang S, Guan Y and Wu X: Astragaloside IV inhibits cell proliferation in vulvar squamous cell carcinoma through the TGF-β/Smad signaling pathway. Dermatol Ther. 32:e128022019. | |
|
Cui X, Jiang X, Wei C, Xing Y and Tong G: Astragaloside IV suppresses development of hepatocellular carcinoma by regulating miR-150-5p/β-catenin axis. Environ Toxicol Pharmacol. 78:1033972020. View Article : Google Scholar | |
|
Ying G: Astragaloside induces gastric MGC-803 cells apoptosis by inhibiting AKT and NF-KB pathway. Int J Lab Med. 19:2341–2344. 2018. | |
|
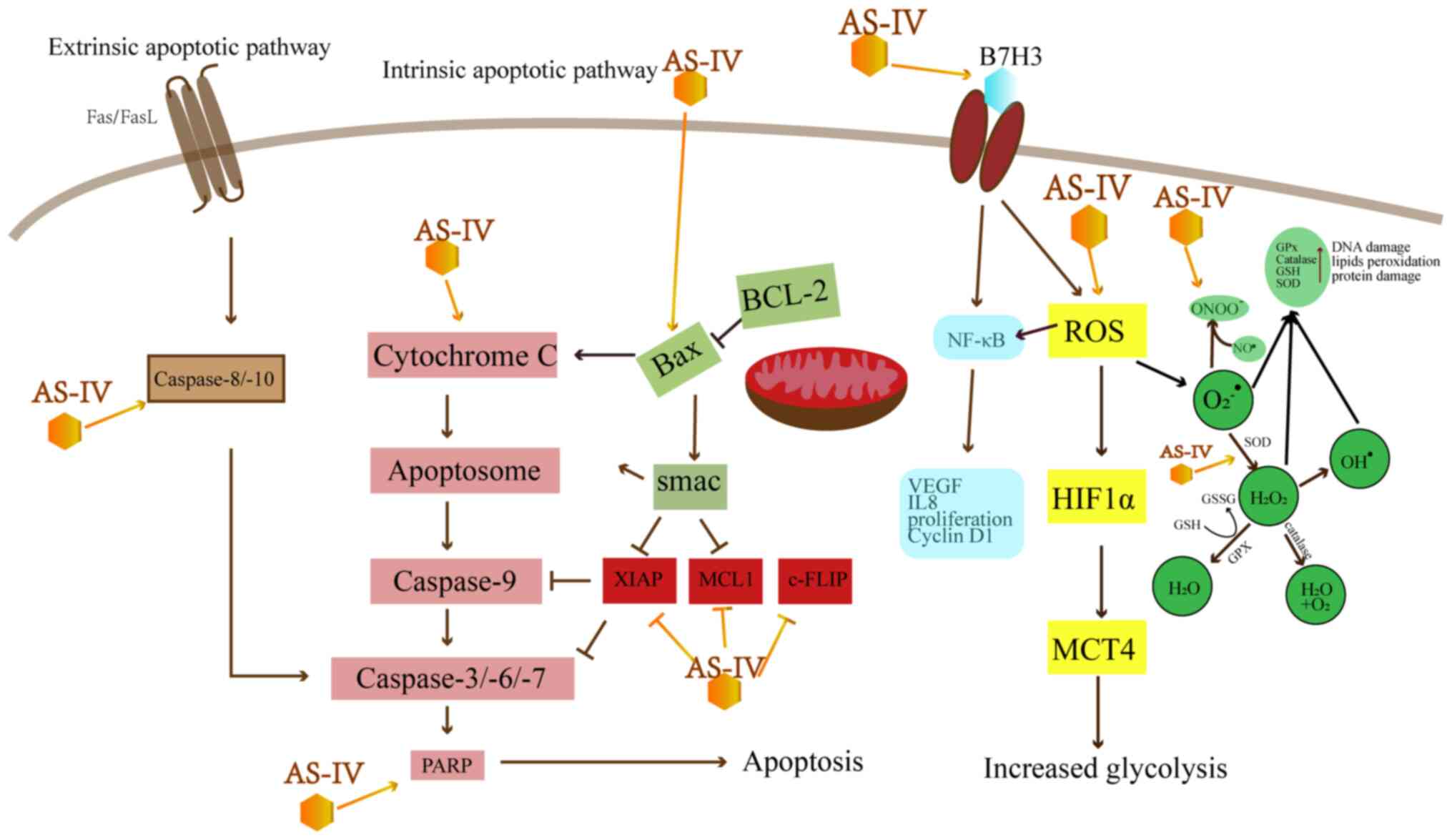
Elmore S: Apoptosis: A review of programmed cell death. Toxicol Pathol. 35:495–516. 2007.PubMed/NCBI | |
|
Hu T, Fei Z and Wei N: Chemosensitive effects of Astragaloside IV in osteosarcoma cells via induction of apoptosis and regulation of caspase-dependent Fas/FasL signaling. Pharmacol Rep. 69:1159–1164. 2017.PubMed/NCBI | |
|
Deveraux QL and Reed JC: IAP family proteins-suppressors of apoptosis. Genes Dev. 13:239–252. 1999.PubMed/NCBI | |
|
Avila MA, Berasain C, Sangro B and Prieto J: New therapies for hepatocellular carcinoma. Oncogene. 25:3866–3884. 2006.PubMed/NCBI | |
|
Du X, Bao G, He X, Zhao H, Yu F, Qiao Q, Lu J and Ma Q: Expression and biological significance of c-FLIP in human hepatocellular carcinomas. J Exp Clin Cancer Res. 28:242009.PubMed/NCBI | |
|
Fleischer B, Schulze-Bergkamen H, Schuchmann M, Weber A, Biesterfeld S, Müller M, Krammer PH and Galle PR: Mcl-1 is an anti-apoptotic factor for human hepatocellular carcinoma. Int J Oncol. 28:25–32. 2006. | |
|
Che Y, Ye F, Xu R, Qing H, Wang X, Yin F, Cui M, Burstein D, Jiang B and Zhang DY: Co-expression of XIAP and cyclin D1 complex correlates with a poor prognosis in patients with hepatocellular carcinoma. Am J Pathol. 180:1798–1807. 2012.PubMed/NCBI | |
|
Cameron BD, Traver G, Roland JT, Brockman AA, Dean D, Johnson L, Boyd K, Ihrie RA and Freeman ML: Bcl2-Expressing Quiescent Type B neural stem cells in the Ventricular-Subventricular zone are resistant to concurrent Temozolomide/X-Irradiation. Stem Cells. 37:1629–1639. 2019.PubMed/NCBI | |
|
Tanaka N, Patel AA, Wang J, Frederick MJ, Kalu NN, Zhao M, Fitzgerald AL, Xie TX, Silver NL, Caulin C, et al: Wee-1 kinase inhibition sensitizes high-risk HPV+ HNSCC to apoptosis accompanied by downregulation of MCl-1 and XIAP antiapoptotic proteins. Clin Cancer Res. 21:4831–4844. 2015.PubMed/NCBI | |
|
Lin YC, Chen RY, Liang JA, Hung YC, Yeh LS, Chang WC, Lin WC, Chang YY and Chen SW: Immunohistochemical biomarkers of survival in patients with adenocarcinoma of the uterine cervix receiving chemoradiotherapy. Anticancer Res. 39:3231–3240. 2019.PubMed/NCBI | |
|
Finkel T: Oxidant signals and oxidative stress. Curr Opin Cell Biol. 15:247–254. 2003.PubMed/NCBI | |
|
Su CM, Wang HC, Hsu FT, Lu CH, Lai CK, Chung JG and Kuo YC: Astragaloside IV induces apoptosis, G1-phase arrest and inhibits anti-apoptotic signaling in hepatocellular carcinoma. In Vivo. 34:631–638. 2020.PubMed/NCBI | |
|
Chang XY: Effects of cisplatin combined with astragaloside iv on apoptosis genes in C6 glioma mice. Chin J Gerontol. 13:3282–3284. 2019.In Chinese. | |
|
Moloney JN and Cotter TG: ROS signalling in the biology of cancer. Semin Cell Dev Biol. 80:50–64. 2018. | |
|
Bułdak RJ, Bułdak Ł, Kukla M, Gabriel A and Zwirska-Korczala K: Significance of selected antioxidant enzymes in cancer cell progression. Pol J Pathol. 65:167–175. 2014. | |
|
Yang JY: Effect of astragaloside IV on the proliferation of Spc-A-1 cells in human lung cancer and its mechanism. Chin Traditional Patent Med. 8:1818–1820. 2016.In Chinese. | |
|
Wang L, Kang FB and Shan BE: B7-H3-mediated tumor immunology: Friend or foe? Int J Cancer. 134:2764–2771. 2014. | |
|
Flem-Karlsen K, Fodstad Ø, Tan M and Nunes-Xavier CE: B7-H3 in cancer - beyond immune regulation. Trends Cancer. 4:401–404. 2018.PubMed/NCBI | |
|
Ling V, Wu PW, Spaulding V, Kieleczawa J, Luxenberg D, Carreno BM and Collins M: Duplication of primate and rodent B7-H3 immunoglobulin V- and C-like domains: Divergent history of functional redundancy and exon loss. Genomics. 82:365–377. 2003.PubMed/NCBI | |
|
Wang S, Mou J, Cui L, Wang X and Zhang Z: Astragaloside IV inhibits cell proliferation of colorectal cancer cell lines through down-regulation of B7-H3. Biomed Pharmacother. 102:1037–1044. 2018. View Article : Google Scholar : PubMed/NCBI | |
|
He CS, Liu YC, Xu ZP, Dai PC, Chen XW and Jin DH: Astragaloside IV enhances cisplatin chemosensitivity in non-small cell lung cancer cells through inhibition of B7-H3. Cell Physiol Biochem. 40:1221–1229. 2016. View Article : Google Scholar : PubMed/NCBI | |
|
An XC: Mechanism of astragaloside IV promoting proliferation and apoptosis of hepatoma cells by inhibiting ROS/NF-κB signaling pathway. Mod Dig Intervent. 12:1399–1403. 2019.In Chinese. | |
|
Brooks PC, Strömblad S, Sanders LC, von Schalscha TL, Aimes RT, Stetler-Stevenson WG, Quigley JP and Cheresh DA: Localization of matrix metalloproteinase MMP-2 to the surface of invasive cells by interaction with integrin alpha v beta 3. Cell. 85:683–693. 1996. View Article : Google Scholar : PubMed/NCBI | |
|
Trepat X, Chen Z and Jacobson K: Cell migration. Compr Physiol. 2:2369–2392. 2012. | |
|
Zhou L, Wang DS, Li QJ, Sun W, Zhang Y and Dou KF: Downregulation of the Notch signaling pathway inhibits hepatocellular carcinoma cell invasion by inactivation of matrix metalloproteinase-2 and -9 and vascular endothelial growth factor. Oncol Rep. 28:874–882. 2012. View Article : Google Scholar : PubMed/NCBI | |
|
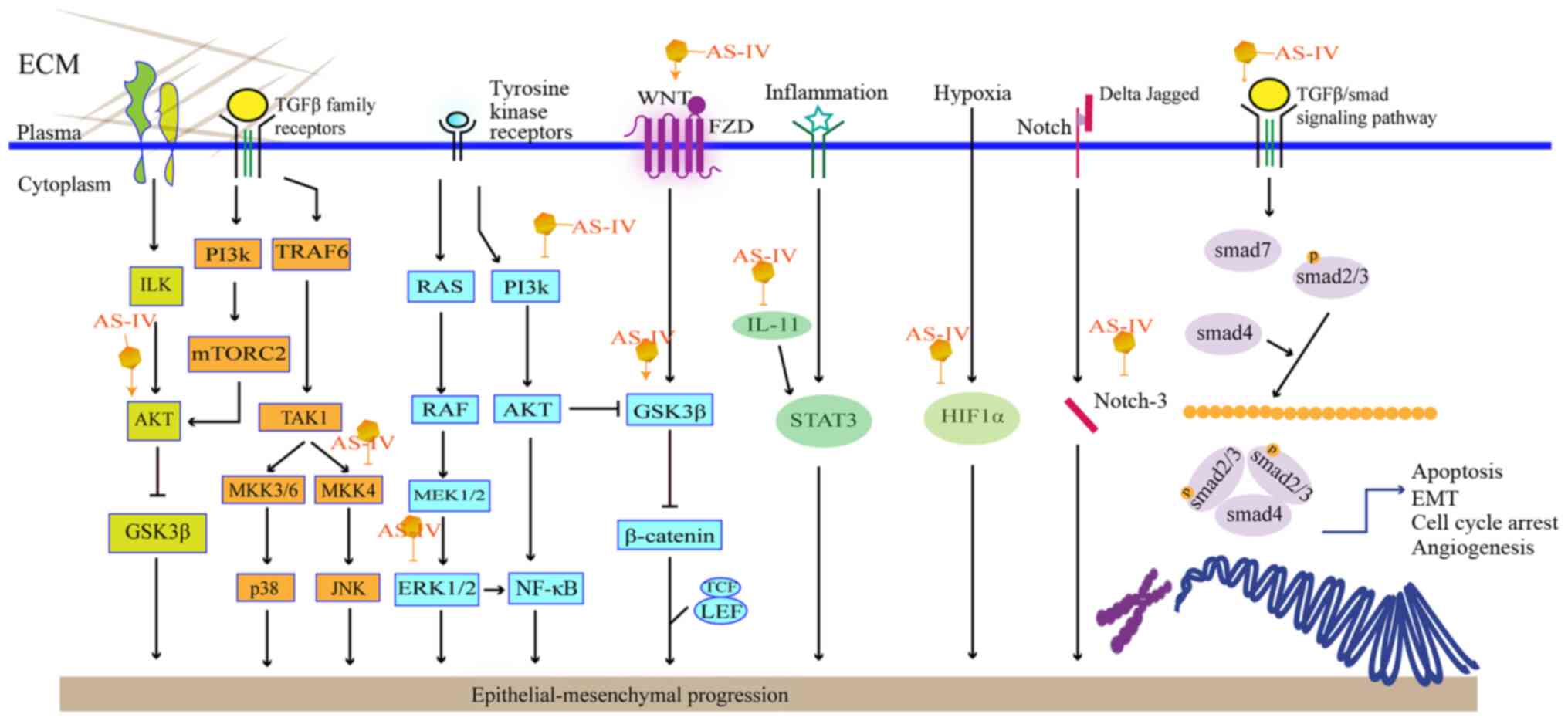
Asati V, Mahapatra DK and Bharti SK: PI3K/Akt/mTOR and Ras/Raf/MEK/ERK signaling pathways inhibitors as anticancer agents: Structural and pharmacological perspectives. Eur J Med Chem. 109:314–341. 2016. View Article : Google Scholar : PubMed/NCBI | |
|
Rizzo D, Ruggiero A, Amato M, Maurizi P and Riccardi R: BRAF and MEK inhibitors in pediatric glioma: New therapeutic strategies, new toxicities. Expert Opin Drug Metab Toxicol. 12:1397–1405. 2016. View Article : Google Scholar : PubMed/NCBI | |
|
Zohrabian VM, Forzani B, Chau Z, Murali R and Jhanwar-Uniyal M: Rho/ROCK and MAPK signaling pathways are involved in glioblastoma cell migration and proliferation. Anticancer Res. 29:119–123. 2009.PubMed/NCBI | |
|
Nickl-Jockschat T, Arslan F, Doerfelt A, Bogdahn U, Bosserhoff A and Hau P: An imbalance between Smad and MAPK pathways is responsible for TGF-beta tumor promoting effects in high-grade gliomas. Int J Oncol. 30:499–507. 2007.PubMed/NCBI | |
|
Wu QN, Liao YF, Lu YX, Wang Y, Lu JH, Zeng ZL, Huang QT, Sheng H, Yun JP, Xie D, et al: Pharmacological inhibition of DUSP6 suppresses gastric cancer growth and metastasis and overcomes cisplatin resistance. Cancer Lett. 412:243–255. 2018. View Article : Google Scholar | |
|
Jiang X, Zhu X, Huang W, Xu H, Zhao Z, Li S, Li S, Cai J and Cao J: Garlic-derived organosulfur compound exerts antitumor efficacy via activation of MAPK pathway and modulation of cytokines in SGC-7901 tumor-bearing mice. Int Immunopharmacol. 48:135–145. 2017. View Article : Google Scholar : PubMed/NCBI | |
|
Li B, Wang F, Liu N, Shen W and Huang T: Astragaloside IV inhibits progression of glioma via blocking MAPK/ERK signaling pathway. Biochem Biophys Res Commun. 491:98–103. 2017. View Article : Google Scholar : PubMed/NCBI | |
|
Cao Y: The anti-invasion effects of astragaloside IV on gastric cancer cell line SGC7901 and its related mechanism. Shanxi Med J. 6:656–659. 2015.In Chinese. | |
|
Wu JY: Inhibition and mechanism of astragaloside IV on H22 ascites in BALB/C mice. Chin J Pharmacovigilance. 3:138–142. 2016.In Chinese. | |
|
Ogata Y, Miura K, Ohkita A, Nagase H and Shirouzu K: Imbalance between matrix metalloproteinase 9 and tissue inhibitor of metalloproteinases 1 expression by tumor cells implicated in liver metastasis from colorectal carcinoma. Kurume Med J. 48:211–218. 2001. View Article : Google Scholar : PubMed/NCBI | |
|
Hajitou A, Sounni NE, Devy L, Grignet-Debrus C, Lewalle JM, Li H, Deroanne CF, Lu H, Colige A, Nusgens BV, et al: Down-regulation of vascular endothelial growth factor by tissue inhibitor of metalloproteinase-2: Effect on in vivo mammary tumor growth and angiogenesis. Cancer Res. 61:3450–3457. 2001.PubMed/NCBI | |
|
Keshavarz-Pakseresht B, Shandiz SA and Baghbani-Arani F: Imatinib induces up-regulation of NM23, a metastasis suppressor gene, in human Hepatocarcinoma (HepG2) cell line. Gastroenterol Hepatol Bed Bench. 10:29–33. 2017.PubMed/NCBI | |
|
Zhou K: Effects of astragaloside IV on gastric cancer cells and its related mechanisms. Hebei Medical University. 2016. | |
|
Du B and Shim JS: Targeting epithelial-mesenchymal transition (EMT) to overcome drug resistance in cancer. Molecules. 21:9652016. View Article : Google Scholar | |
|
Han J, Shen X, Zhang Y, Wang S and Zhou L: Astragaloside IV suppresses transforming growth factor-β1-induced epithelial-mesenchymal transition through inhibition of Wnt/β-catenin pathway in glioma U251 cells. Biosci Biotechnol Biochem. 84:1345–1352. 2020. View Article : Google Scholar : PubMed/NCBI | |
|
Larue L and Bellacosa A: Epithelial-mesenchymal transition in development and cancer: Role of phosphatidylinositol 3′ kinase/AKT pathways. Oncogene. 24:7443–7454. 2005. View Article : Google Scholar : PubMed/NCBI | |
|
Qin CD, Ma DN, Ren ZG, Zhu XD, Wang CH, Wang YC, Ye BG, Cao MQ, Gao DM and Tang ZY: Astragaloside IV inhibits metastasis in hepatoma cells through the suppression of epithelial-mesenchymal transition via the Akt/GSK-3β/β-catenin pathway. Oncol Rep. 37:1725–1735. 2017. View Article : Google Scholar : PubMed/NCBI | |
|
Zhang L, Zhou J, Qin X, Huang H and Nie C: Astragaloside IV inhibits the invasion and metastasis of SiHa cervical cancer cells via the TGF-β1-mediated PI3K and MAPK pathways. Oncol Rep. 41:2975–2986. 2019.PubMed/NCBI | |
|
Cheng X, Gu J, Zhang M, Yuan J, Zhao B, Jiang J and Jia X: Astragaloside IV inhibits migration and invasion in human lung cancer A549 cells via regulating PKC-α-ERK1/2-NF-κB pathway. Int Immunopharmacol. 23:304–313. 2014. View Article : Google Scholar : PubMed/NCBI | |
|
Su CC, Chiou TL, Chan MH and Lin JG: Astragaloside IV increases MMP-2 mRNA and protein expression in human lung cancer A549 cells. Mol Med Rep. 2:107–113. 2009.PubMed/NCBI | |
|
Liu YN, Yin JJ, Abou-Kheir W, Hynes PG, Casey OM, Fang L, Yi M, Stephens RM, Seng V, Sheppard-Tillman H, et al: MiR-1 and miR-200 inhibit EMT via Slug-dependent and tumorigenesis via Slug-independent mechanisms. Oncogene. 32:296–306. 2013. View Article : Google Scholar | |
|
Kitamura K, Seike M, Okano T, Matsuda K, Miyanaga A, Mizutani H, Noro R, Minegishi Y, Kubota K and Gemma A: MiR-134/487b/655 cluster regulates TGF-β-induced epithelial-mesenchymal transition and drug resistance to gefitinib by targeting MAGI2 in lung adenocarcinoma cells. Mol Cancer Ther. 13:444–453. 2014. View Article : Google Scholar | |
|
Liu Y, Zhang M, Qian J, Bao M, Meng X, Zhang S, Zhang L, Zhao R, Li S, Cao Q, et al: miR-134 functions as a tumor suppressor in cell proliferation and epithelial-to-mesenchymal Transition by targeting KRAS in renal cell carcinoma cells. DNA Cell Biol. 34:429–436. 2015. View Article : Google Scholar : PubMed/NCBI | |
|
Ye Q, Su L, Chen D, Zheng W and Liu Y: Astragaloside IV Induced miR-134 expression reduces EMT and increases chemotherapeutic sensitivity by suppressing CREB1 signaling in colorectal cancer cell line SW-480. Cell Physiol Biochem. 43:1617–1626. 2017. View Article : Google Scholar : PubMed/NCBI | |
|
Lin A, Hu Q, Li C, Xing Z, Ma G, Wang C, Li J, Ye Y, Yao J, Liang K, et al: The LINK-A lncRNA interacts with PtdIns(3,4,5) P3 to hyperactivate AKT and confer resistance to AKT inhibitors. Nat Cell Biol. 19:238–251. 2017. View Article : Google Scholar : PubMed/NCBI | |
|
Yan X, Hu Z, Feng Y, Hu X, Yuan J, Zhao SD, Zhang Y, Yang L, Shan W, He Q, et al: Comprehensive genomic characterization of long non-coding RNAs across human cancers. Cancer Cell. 28:529–540. 2015. View Article : Google Scholar : PubMed/NCBI | |
|
Yuan JH, Yang F, Wang F, Ma JZ, Guo YJ, Tao QF, Liu F, Pan W, Wang TT, Zhou CC, et al: A long noncoding RNA activated by TGF-beta promotes the invasion-metastasis cascade in hepatocellular carcinoma. Cancer Cell. 25:666–681. 2014. View Article : Google Scholar : PubMed/NCBI | |
|
Li Y, Ye Y and Chen H: Astragaloside IV inhibits cell migration and viability of hepatocellular carcinoma cells via suppressing long noncoding RNA ATB. Biomed Pharmacother. 99:134–141. 2018. View Article : Google Scholar : PubMed/NCBI | |
|
Jiang K, Lu Q, Li Q, Ji Y, Chen W and Xue X: Astragaloside IV inhibits breast cancer cell invasion by suppressing Vav3 mediated Rac1/MAPK signaling. Int Immunopharmacol. 42:195–202. 2017. View Article : Google Scholar | |
|
Qi H, Wei L, Han Y, Zhang Q, Lau AS and Rong J: Proteomic characterization of the cellular response to chemopreventive triterpenoid astragaloside IV in human hepatocellular carcinoma cell line HepG2. Int J Oncol. 36:725–735. 2010.PubMed/NCBI | |
|
Apte RS, Chen DS and Ferrara N: VEGF in signaling and disease: Beyond discovery and development. Cell. 176:1248–1264. 2019. View Article : Google Scholar : PubMed/NCBI | |
|
Hashemi Goradel N, Najafi M, Salehi E, Farhood B and Mortezaee K: Cyclooxygenase-2 in cancer: A review. J Cell Physiol. 234:5683–5699. 2019. View Article : Google Scholar | |
|
Cao LP: Mod J Integr Tradit Chin West Med. 7:798–800. 2010.In Chinese. | |
|
Li YJ, Lei YH, Yao N, Wang CR, Hu N, Ye WC, Zhang DM and Chen ZS: Autophagy and multidrug resistance in cancer. Chin J Cancer. 36:522017. View Article : Google Scholar : PubMed/NCBI | |
|
Choi YH and Yu AM: ABC transporters in multidrug resistance and pharmacokinetics, and strategies for drug development. Curr Pharm Des. 20:793–807. 2014. View Article : Google Scholar | |
|
Wang PP, Luan JJ, Xu WK, Wang L, Xu DJ, Yang CY, Zhu YH and Wang YQ: Astragaloside IV downregulates the expression of MDR1 in Bel-7402/FU human hepatic cancer cells by inhibiting the JNK/c-Jun/AP-1 signaling pathway. Mol Med Rep. 16:2761–2766. 2017. View Article : Google Scholar : PubMed/NCBI | |
|
Wang PP, Xu DJ, Huang C, Wang WP and Xu WK: Astragaloside IV reduces the expression level of P-glycoprotein in multi-drug-resistant human hepatic cancer cell lines. Mol Med Rep. 9:2131–2137. 2014. View Article : Google Scholar : PubMed/NCBI | |
|
Sebastián C, Zwaans BM, Silberman DM, Gymrek M, Goren A, Zhong L, Ram O, Truelove J, Guimaraes AR, Toiber D, et al: The histone deacetylase SIRT6 is a tumor suppressor that controls cancer metabolism. Cell. 151:1185–1199. 2012. View Article : Google Scholar : PubMed/NCBI | |
|
Dai PC, Liu DL, Zhang L, Ye J, Wang Q, Zhang HW, Lin XH and Lai GX: Astragaloside IV sensitizes non-small cell lung cancer cells to gefitinib potentially via regulation of SIRT6. Tumour Biol. 39:10104283176975552017. View Article : Google Scholar : PubMed/NCBI | |
|
Xie T, Li Y, Li SL and Luo HF: Astragaloside IV enhances cisplatin chemosensitivity in human colorectal cancer via regulating NOTCH3. Oncol Res. 24:447–453. 2016. View Article : Google Scholar | |
|
Tian YZ: The function and mechanism of astragaloside IV on the chemoresistance of HepG2/GCS cell lines. Chin J Hepatobiliary Surg. 8:555–559. 2018.In Chinese. | |
|
Wang Z, Wang N, Liu P, Peng F, Tang H, Chen Q, Xu R, Dai Y, Lin Y, Xie X, et al: Caveolin-1, a stress-related oncotarget, in drug resistance. Oncotarget. 6:37135–37150. 2015. View Article : Google Scholar : PubMed/NCBI | |
|
Morrison DK: MAP kinase pathways. Cold Spring Harb Perspect Biol. 4:a0112542012. View Article : Google Scholar : PubMed/NCBI | |
|
Iachettini S, Trisciuoglio D, Rotili D, Lucidi A, Salvati E, Zizza P, Di Leo L, Del Bufalo D, Ciriolo MR, Leonetti C, et al: Pharmacological activation of SIRT6 triggers lethal autophagy in human cancer cells. Cell Death Dis. 9:9962018. View Article : Google Scholar : PubMed/NCBI | |
|
Shang JL, Ning SB, Chen YY, Chen TX and Zhang J: MDL-800, an allosteric activator of SIRT6, suppresses proliferation and enhances EGFR-TKIs therapy in non-small cell lung cancer. Acta Pharmacol Sin. 42:120–131. 2021. View Article : Google Scholar | |
|
Krishnamoorthy V and Vilwanathan R: Silencing Sirtuin 6 induces cell cycle arrest and apoptosis in non-small cell lung cancer cell lines. Genomics. 112:3703–3712. 2020. View Article : Google Scholar : PubMed/NCBI | |
|
Wang J, Cai Y and Sheng Z: Experimental studies on the protective effects of the overexpression of lentivirus-mediated sirtuin 6 on radiation-induced lung injury. Adv Clin Exp Med. 29:873–877. 2020. View Article : Google Scholar : PubMed/NCBI | |
|
Giovannini C, Baglioni M, Baron Toaldo M, Ventrucci C, D'Adamo S, Cipone M, Chieco P, Gramantieri L and Bolondi L: Notch3 inhibition enhances sorafenib cytotoxic efficacy by promoting GSK3b phosphorylation and p21 down-regulation in hepatocellular carcinoma. Oncotarget. 4:1618–1631. 2013. View Article : Google Scholar : PubMed/NCBI | |
|
Giovannini C, Gramantieri L, Chieco P, Minguzzi M, Lago F, Pianetti S, Ramazzotti E, Marcu KB and Bolondi L: Selective ablation of Notch3 in HCC enhances doxorubicin's death promoting effect by a p53 dependent mechanism. J Hepatol. 50:969–979. 2009. View Article : Google Scholar : PubMed/NCBI | |
|
Liu YY, Hill RA and Li YT: Ceramide glycosylation catalyzed by glucosylceramide synthase and cancer drug resistance. Adv Cancer Res. 117:59–89. 2013. View Article : Google Scholar : PubMed/NCBI | |
|
Farhood B, Najafi M and Mortezaee K: CD8(+) cytotoxic T lymphocytes in cancer immunotherapy: A review. J Cell Physiol. 234:8509–8521. 2019. View Article : Google Scholar | |
|
Zhang A, Zheng Y, Que Z, Zhang L, Lin S, Le V, Liu J and Tian J: Astragaloside IV inhibits progression of lung cancer by mediating immune function of Tregs and CTLs by interfering with IDO. J Cancer Res Clin Oncol. 140:1883–1890. 2014. View Article : Google Scholar : PubMed/NCBI | |
|
Xu F, Cui WQ, Wei Y, Cui J, Qiu J, Hu LL, Gong WY, Dong JC and Liu BJ: Astragaloside IV inhibits lung cancer progression and metastasis by modulating macrophage polarization through AMPK signaling. J Exp Clin Cancer Res. 37:2072018. View Article : Google Scholar : PubMed/NCBI | |
|
Liu TG: Effects of cisplatin combined with astragaloside IV on inflammatory factors and immune function in rats with breast cancer. Chin J Gerontol. 4:863–865. 2020.In Chinese. | |
|
Lin L: The antitumor effect ASIV and β-elemene to the immune system of mice with liver tumor. Nanjing University of Chinese Medicine. 2011. | |
|
Li Y, Meng T, Hao N, Tao H, Zou S, Li M, Ming P, Ding H, Dong J, Feng S, et al: Immune regulation mechanism of Astragaloside IV on RAW264.7 cells through activating the NF-κB/MAPK signaling pathway. Int Immunopharmacol. 49:38–49. 2017. View Article : Google Scholar : PubMed/NCBI | |
|
Singh SS, Vats S, Chia AY, Tan TZ, Deng S, Ong MS, Arfuso F, Yap CT, Goh BC, Sethi G, et al: Dual role of autophagy in hall-marks of cancer. Oncogene. 37:1142–1158. 2018. View Article : Google Scholar | |
|
Tanida I, Ueno T and Kominami E: LC3 and Autophagy. Methods Mol Biol. 445:77–88. 2008. View Article : Google Scholar : PubMed/NCBI | |
|
Xia C, He Z and Cai Y: Quantitative proteomics analysis of differentially expressed proteins induced by astragaloside IV in cervical cancer cell invasion. Cell Mol Biol Lett. 25:252020. View Article : Google Scholar : PubMed/NCBI | |
|
Hong CS, Graham NA, Gu W, Espindola Camacho C, Mah V, Maresh EL, Alavi M, Bagryanova L, Krotee PAL, Gardner BK, et al: MCT1 modulates cancer cell pyruvate export and growth of tumors that co-express MCT1 and MCT4. Cell Rep. 14:1590–1601. 2016. View Article : Google Scholar : PubMed/NCBI | |
|
Zhang C, Cai T, Zeng X, Cai D, Chen Y, Huang X, Gan H, Zhuo J, Zhao Z, Pan H and Li S: Astragaloside IV reverses MNNG-induced precancerous lesions of gastric carcinoma in rats: Regulation on glycolysis through miRNA-34a/LDHA pathway. Phytother Res. 32:1364–1372. 2018. View Article : Google Scholar : PubMed/NCBI | |
|
Wang ZF, Ma DG, Zhu Z, Mu YP, Yang YY, Feng L, Yang H, Liang JQ, Liu YY, Liu L and Lu HW: Astragaloside IV inhibits pathological functions of gastric cancer-associated fibroblasts. World J Gastroenterol. 23:8512–8525. 2017. View Article : Google Scholar | |
|
Lou H, Kaur K, Sharma AK and Singal PK: Adriamycin-induced oxidative stress, activation of MAP kinases and apoptosis in isolated cardiomyocytes. Pathophysiology. 13:103–109. 2006. View Article : Google Scholar : PubMed/NCBI | |
|
Cave A: Selective targeting of NADPH oxidase for cardiovascular protection. Curr Opin Pharmacol. 9:208–213. 2009. View Article : Google Scholar | |
|
Lin J, Fang L, Li H, Li Z, Lyu L, Wang H and Xiao J: Astragaloside IV alleviates doxorubicin induced cardiomyopathy by inhibiting NADPH oxidase derived oxidative stress. Eur J Pharmacol. 859:1724902019. View Article : Google Scholar : PubMed/NCBI | |
|
Lou Y, Guo Z, Zhu Y, Zhang G, Wang Y, Qi X, Lu L, Liu Z and Wu J: Astragali radix and its main bioactive compounds activate the Nrf2-mediated signaling pathway to induce P-glycoprotein and breast cancer resistance protein. J Ethnopharmacol. 228:82–91. 2019. View Article : Google Scholar | |
|
Zhu J and Wen K: Astragaloside IV inhibits TGF-β1-induced epithelial-mesenchymal transition through inhibition of the PI3K/Akt/NF-κB pathway in gastric cancer cells. Phytother Res. 32:1289–1296. 2018. View Article : Google Scholar : PubMed/NCBI | |
|
Zhang G, Ou R, Li F, Wu J, Zheng L, Tong Y, Liu Y, Liu Z and Lu L: Regulation of drug-metabolizing enzymes and efflux transporters by Astragali radix decoction and its main bioactive compounds: Implication for clinical drug-drug interactions. J Ethnopharmacol. 180:104–113. 2016. View Article : Google Scholar : PubMed/NCBI |