A pilot study on the safety and efficacy of neoadjuvant chemo‑adoptive immunotherapy for locally advanced rectal cancer
- Authors:
- Published online on: January 15, 2024 https://doi.org/10.3892/ol.2024.14234
- Article Number: 101
-
Copyright: © Okazawa et al. This is an open access article distributed under the terms of Creative Commons Attribution License.
Abstract
Introduction
In Europe and in the United States, total mesorectal excision (TME) or tumor-specific mesorectal excision is the standard treatment after neoadjuvant chemoradiotherapy (NACRT) for locally advanced rectal cancer (LARC). However, NACRT has not been shown to improve overall survival (OS) or prognosis because, although it reduces the local recurrence (LR) rate (range, 5.6–9%), it does not reduce the multi-organ metastasis rate (30%) (1–4). Neoadjuvant chemotherapy (NAC) can be considered to avoid adverse events associated with radiation therapy and improve survival rates by controlling distant metastases. However, generally, NAC is considered to have a higher LR rate than NACRT, and there are still insufficient data on NAC. Hence, NAC is considered insufficient to prevent LR in cT4b cases (5). To overcome these issues, total NAC, which applies systemic chemotherapy before rather than after surgery, has gained attention (6).
In recent years, cancer immunotherapy, particularly immune checkpoint inhibitors (ICIs), have been used to treat various types of solid tumors such as hepatocellular carcinoma and lung cancer (7,8). Adaptive immune cell therapies, such as tumor-infiltrating lymphocyte (TIL) therapy for melanoma and chimeric antigen receptor-T cell therapy for hematological malignancies, have also been used (9,10). Immune cell therapy exerts antitumor properties through a mechanism of action that is different from that of chemo- and radiotherapy, where LAK cells mediate potent tumor cytolysis without MHC restrictions independent of the tumor type (11). Positive outcomes are expected when immune cell therapy is used in combination with other therapies such as chemotherapy (12). αβ T-lymphocyte therapy is a method involving notable proliferation and activation of all lymphocytes, such as T and NK cells, that target cancer cells and raise overall immunity. The safety and efficacy of chemo-adoptive immunotherapy (CAIT) for patients with stage IV or recurrent colorectal cancer have been previously reported (12). Results showed the median progression-free survival was 21.3 months, the response rate was 80% [complete response (CR), 26.7%; partial response (PR), 53.3%], and with almost no adverse events. However, the significance and mechanism of CAIT have not been sufficiently evaluated.
Therefore, the safety and efficacy of neoadjuvant CAIT for LARC was investigated in the present study. In addition, to explore the mechanism of CAIT, the changes in immune cells in the peripheral blood and in the tumor microenvironment were studied.
Patients and methods
Study design
The present study is a prospective, non-randomized, open-label, single-arm, translational clinical trial carried out in Japan, and performed in accordance with ethical guidelines for clinical studies. The Institutional Review Board (IRB) of Juntendo University approved the protocol, and the current study was registered with the Japan Registry of Clinical Trials (jRCT; ID, jRCTc030190248; January 21, 2019). The present study was reviewed and approved by the relevant Accreditation Committee for Regenerative Medicine (Tokyo, Japan). The IRBs of all participating institutions approved the present clinical study (Juntendo University, Tokyo, Japan; approval no. 2018061; Nippon Medical School Tokyo, Japan; approval no. 2018-212), and written informed consent was obtained from every patient. Patient registration required approval from the ethics committees of all participating medical institutions, but no patients were registered at Fukuoka University Hospital.
The safety of neoadjuvant CAIT for LARC was investigated as a primary endpoint. In addition, efficacy and immunological response were evaluated as secondary endpoints. The target sample size was six patients because this was a feasibility study, and the sample size was not calculated.
Patient selection
Four patients were enrolled between March 2019 and January 2020 from Juntendo University, and two patients were enrolled between February and July 2020 from Nippon Medical School. Eligible patients were ≥20 and ≤80 years old, had histologically confirmed rectal adenocarcinoma without prior chemo or radiotherapy for any other cancers, had ≥cT3 stage or had local metastases to lymph nodes but no distant metastasis and no direct invasion into the trigone bladder, urethra or sacrum (13). Rectum was defined as the distance from the second sacral vertebra to the upper edge of the anal canal. Those patients who met the following criteria were included in the present study: i) Eastern Cooperative Oncology Group performance status (ECOG PS) score range, 0–1; ii) neutrophil count, ≥1,500/mm3; iii) platelet count, ≥100,000/mm3; iv) total bilirubin, ≤2.0 mg/dl; v) aspartate transferase and alanine transferase, ≤100 IU/l; and vi) serum creatinine, ≤1.5 mg/dl. Patients were excluded based on the following exclusion criteria: i) Multiple primary cancers within the past 5 years; ii) active infection; iii) positive human immunodeficiency virus or human T-cell lymphotropic virus type I test result; iv) positive microsatellite instability test; v) systemic steroid or immunosuppressant administration; vi) pregnancy; vii) uncontrolled diabetes; viii) interstitial lung disease; ix) autoimmune disease; x) clinically significant cardiovascular disease; and xi) any other conditions that made the patient unsuitable for inclusion in the present study (14).
Treatment of neoadjuvant CAIT
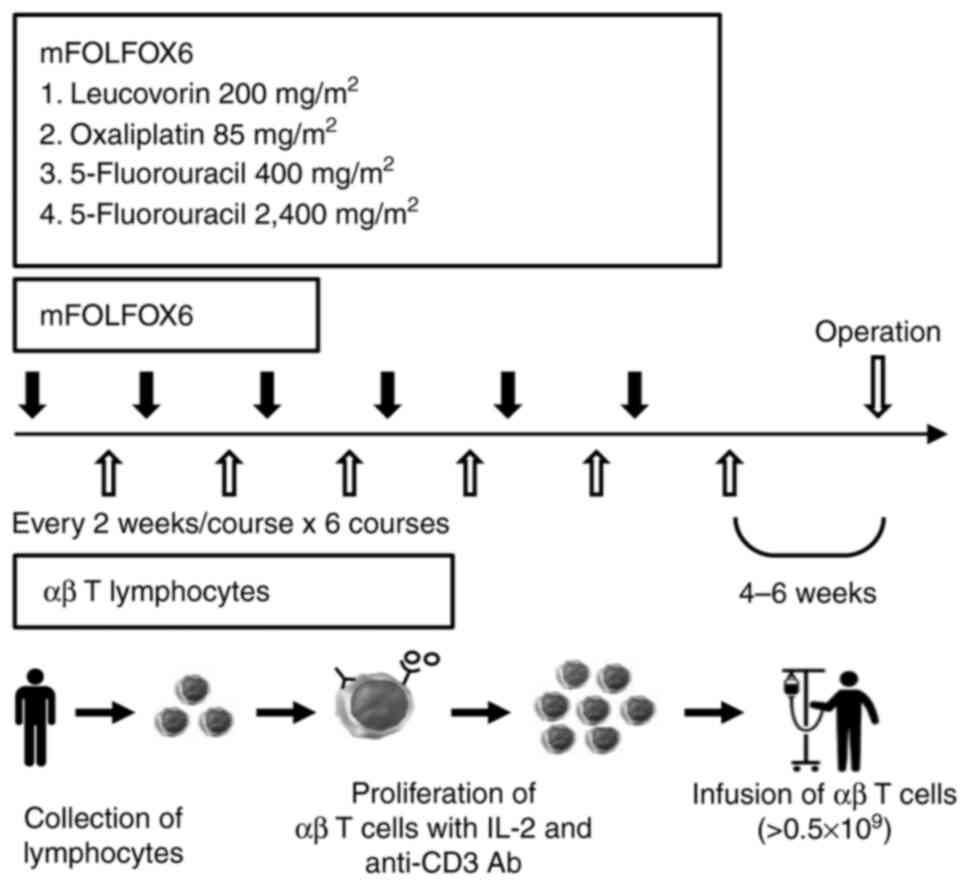
ChemotherapyFor advanced rectal cancer, patients received a FOLFOX6 protocol composed of 85 mg/m2oxaliplatin, 200 mg/m2 leucovorin and 400 mg/m2 fluorouracil as an intravenous bolus with a 46-h continuous injection of 2,400 mg/m2 fluorouracil on day 1. Patients were administered six courses of this therapy every 2 weeks.
Immunotherapy
Peripheral blood mononuclear cells (PBMCs) were harvested using a Vacutainer (Becton, Dickinson and Company) by centrifugation at 1,500 × g at 4°C for 15 min. A total of ≥0.5×109 αβ T-lymphocytes were cultured ex vivo with an immobilized antibody to CD3 (muromonab-CD3; Janssen-Cilag Ltd.; Johnson & Johnson) in a medium containing 1% autologous serum at 37°C in a 5% CO2 incubator, then cultured in the presence of 700 IU/ml recombinant interleukin-2 (Proleukin®; Novartis International) for 9 days, and finally injected intravenously into patients once every 2 weeks, starting 10 days after mFOLFOX6 therapy initiation. Surface antigen analysis of the injected cells by flow cytometry (FCM) in FACS Calibur (Becton, Dickinson and Company) using the FITC-conjugated antibody to CD8 (clone SK1; BioLegend, Inc.) showed that CD8+ T cells were the most cultured (range, 48.1–78.7%; data not shown). Surgery was performed 4–6 weeks after the last αβ T lymphocyte injection (Fig. 1).
Evaluation of toxicity and efficacy of neoadjuvant CAIT
Evaluation of toxicity of neoadjuvant CAITSafety was evaluated by assessment of all adverse events, laboratory data, symptoms, objective findings, body weight, ECOG-PS score, imaging findings and postoperative complications. Adverse events were evaluated according to the National Institute Common Terminology Criteria for Adverse Events version 4.0 (15). Laboratory and adverse event monitoring were performed before all cycles of CAIT. Treatment was delayed if any of the following were noted on the day of administration: i) Neutrophil count, <1,000/mm3; ii) platelet count, <75,000/mm3; iii) active infection with fever ≥38.0°C; iv) ≥grade 2 peripheral sensory neuropathy (PSN); and v) ≥grade 3 non-hematological toxicity. The oxaliplatin dose was reduced to 65 mg/m2 if grade 3–4 neutropenia, febrile neutropenia or thrombocytopenia, persistent grade 2 or reversible grade 3 PSN, or any grade 3–4 non-hematological toxicity occurred. The continuous fluorouracil dose was reduced to 2,000 mg/m2 if grade 4 neutropenia, grade 3–4 febrile neutropenia or thrombocytopenia, or if any grade 3–4 non-hematological toxicity occurred. The present study was terminated if grade 3 toxicity persisted after oxaliplatin dose reduction to 50 mg/m2, continuous injection of 1,600 mg/m2 fluorouracil, or if grade 4 non-hematological toxicities occurred.
Evaluation of efficacy of neoadjuvant CAIT
All patients underwent a physical examination; computed tomography (CT) scans of the chest, abdomen and pelvis, and magnetic resonance imaging (MRI) of the abdomen and pelvis before and after neoadjuvant CAIT were performed. Effects were evaluated by the reduction ratio of tumors, downstaging rate, histopathological effect, immunopathological effect and prognosis. After the completion of neoadjuvant CAIT, the maximum tumor thickness was measured by MRI, and the reduction ratio was evaluated according to the Response Evaluation Criteria for Solid Tumors (RECIST) criteria version 1.1 (16). The preoperative reduction ratio was calculated as the percentage of eligible patients with measurable lesions who achieved either CR or PR according to RECIST criteria. Cancer staging was evaluated using the TNM classification version 8 (13). Downstaging was defined as the reduction in pathological T and N stages from the clinical stage. Histopathological effects were evaluated according to the Japanese Classification of Colorectal, Appendiceal and Anal Carcinoma guidelines (3rd English edition) (17). According to the guidelines, grades 0, 1a, 1b, 2 and 3 indicated no effect, and minimal, mild, moderate and marked effect, respectively (17).
Assessment of immunological status in the peripheral blood
Assessment of patient immunological status and injected immune cellsThe number and frequency of immune cells in peripheral blood samples were examined by FCM from patients before and after treatment as previously reported (18). The phenotype of PBMCs was analyzed using monoclonal antibodies (mAbs) against CD3, CD4, CD8, CD45, CD56, T cell receptor (TCR) PAN αβ, TCR PAN γδ and TCRVγ9 (Beckman Coulter, Inc.). The isolated PBMCs were used for Foxp3 staining and cytokine production assays. For Foxp3 staining, Foxp3 was stained with an anti-Foxp3 mAb (clone 259D; BioLegend, Inc.) after cell fixation and permeabilization. For the intracellular cytokine production assay, activated cells were fixed, permeabilized and then the intracellular cytokines were stained with anti-IFN-γ or -IL-4 mAbs (Beckman Coulter, Inc.).
Immunohistochemical analysis of tumor infiltrating lymphocytes (TILs)
TILs in tumor tissue were evaluated by immunohistochemical analysis, as previously reported (19). TILs were compared between biopsy tissue collected endoscopically pre- and post-CAIT. TILs were stained with anti-human CD3, CD4, CD8 and CD56 mAbs (clones PS1, 4B12, 4B11 and ERIC1, respectively; Novocastra Laboratories Ltd.) and anti-human FOXP3 mAb (clone 236A/E7; eBioscience; Thermo Fisher Scientific, Inc.). Sections with a thickness of 3 µm were incubated with primary antibodies diluted 100–200× at room temperature for 15 min for CD3, CD4, and CD8 and overnight for CD56 and Foxp3. After washing with phosphate buffer containing Tween 20, tumor sections were incubated with HRP-labeled anti-IgG Ab (Nichirei Biosciences, Inc.) for 10–30 min, and each positive cell was detected with 3,3′-diaminobenzidine, tetra-hydrochloride. The number of cells positive for each TIL out of 1,000 lymphocytes was measured to calculate the positive rate, in %, for every TIL.
Statistical analysis
Statistical analysis was performed using the unpaired Student's t-test for analysis of changes in immune cell counts, and P<0.05 was considered to indicate a statistically significant difference.
Results
Patient characteristics
At Juntendo University, four males (49, 51, 54 and 63 years old, respectively) were enrolled, and at Nippon Medical School, a 76-year-old male patient and a 63-year-old female patient were enrolled. The ECOG PS score was 0 for all patients. Four patients had upper rectal carcinoma and two had lower rectal carcinoma.
Treatment with neoadjuvant CAIT
ChemotherapyAll six patients completed the six planned cycles. One patient (16.7%) discontinued oxaliplatin due to an allergic reaction in the 6th cycle. Two patients (33.3%) required a dose reduction of oxaliplatin because of peripheral neuropathy or neutropenia. One patient (16.6%) required a dose reduction of fluorouracil due to liver dysfunction. The median relative dose intensity of bolus fluorouracil was 100% (range, 88–100%), of continuous infusion of fluorouracil was 100% (range, 94.4–100%) and of oxaliplatin was 98% (range, 94.4–100%).
Immunotherapy
All six patients completed the six planned cycles. The mean number of cells for each infusion was 5.0×109 cells (range, 1.4–7.8×109 cells).
Safety
The adverse events in the six patients are summarized in Table I. Only one patient (16.7%) developed grade 3 hematological toxicity (neutropenia). No patient experienced ≥grade 3 non-hematological toxicity. One patient experienced grade 2 hypocalcemia due to apheresis. No other severe treatment-related adverse events or deaths were recorded during treatment.
Efficacy
The median reduction rate was 30.5% (range, 18–40%). The confirmed response rate was 66.7% [CR, 0%; PR, 66.7% (n=4); stable disease (SD), 33.3% (n=2); progressive disease (PD), 0%] and the disease control rate (CR + PR + SD) was 100%. Downstaging was confirmed in five patients (83%). Regarding histological effects, two patients were grade 1a, and four were grade 2 (Table II). The clinical stage before preoperative treatment (cStage), clinical stage after preoperative treatment (ycStage) and postoperative pathologic stage (ypStage) of the six patients are shown in Table II (13).
Table II.Effect of neoadjuvant chemo-adaptive immunotherapy, surgical procedure and postoperative course. |
Surgical procedure and short-term outcomes
The surgical approaches included robot-assisted surgery in four cases and laparoscopic surgery in two cases. The surgical procedure was low anterior resection in four cases, intersphincteric resection in one case and abdominoperineal resection in one case. Bilateral lymph node dissection was performed in four cases. R0 resection was achieved in all the cases. R0 resection was defined as no evidence of tumor at the surgical margin, macroscopically or pathologically. Regarding postoperative complications, grades 2 and 3b outlet obstructions were observed in two patients (one each), and grade 2 renal dysfunction due to excessive stoma drainage and grade 1 anastomotic leakage were observed in one case. Postoperative adjuvant chemotherapy was administered in three patients. The median follow-up duration was 24 months. Liver and pulmonary metastases were observed in one patient 13 months after radical resection surgery following neoadjuvant chemo--adoptive immunotherapy, and the remaining five patients had no recurrence (Table II).
Immunological assessment of immune cells in the peripheral blood and tumors
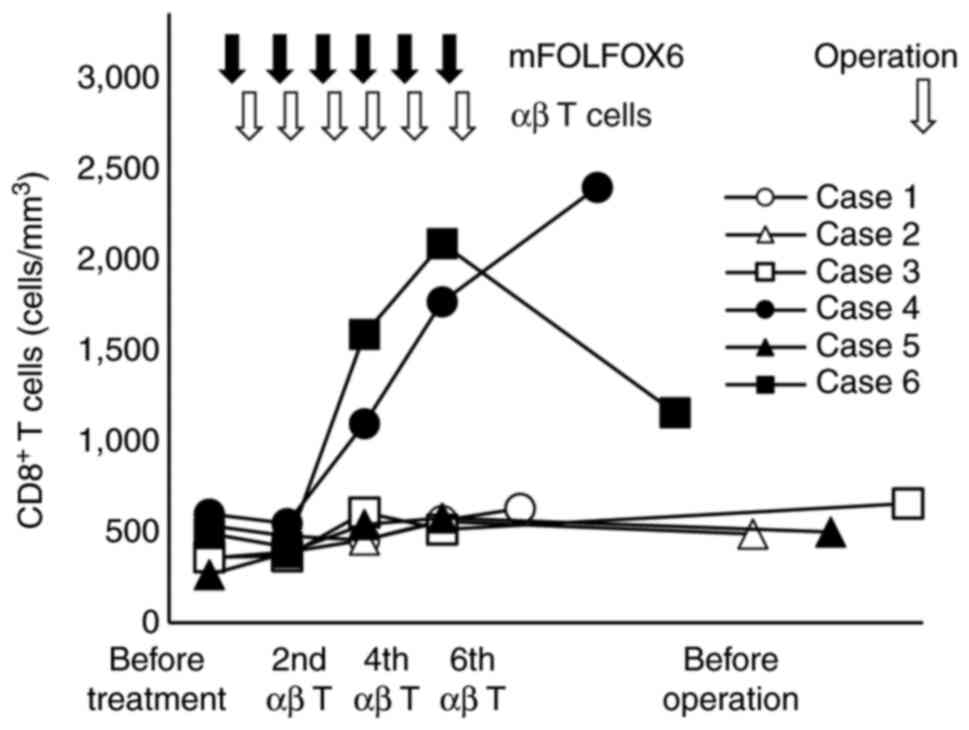
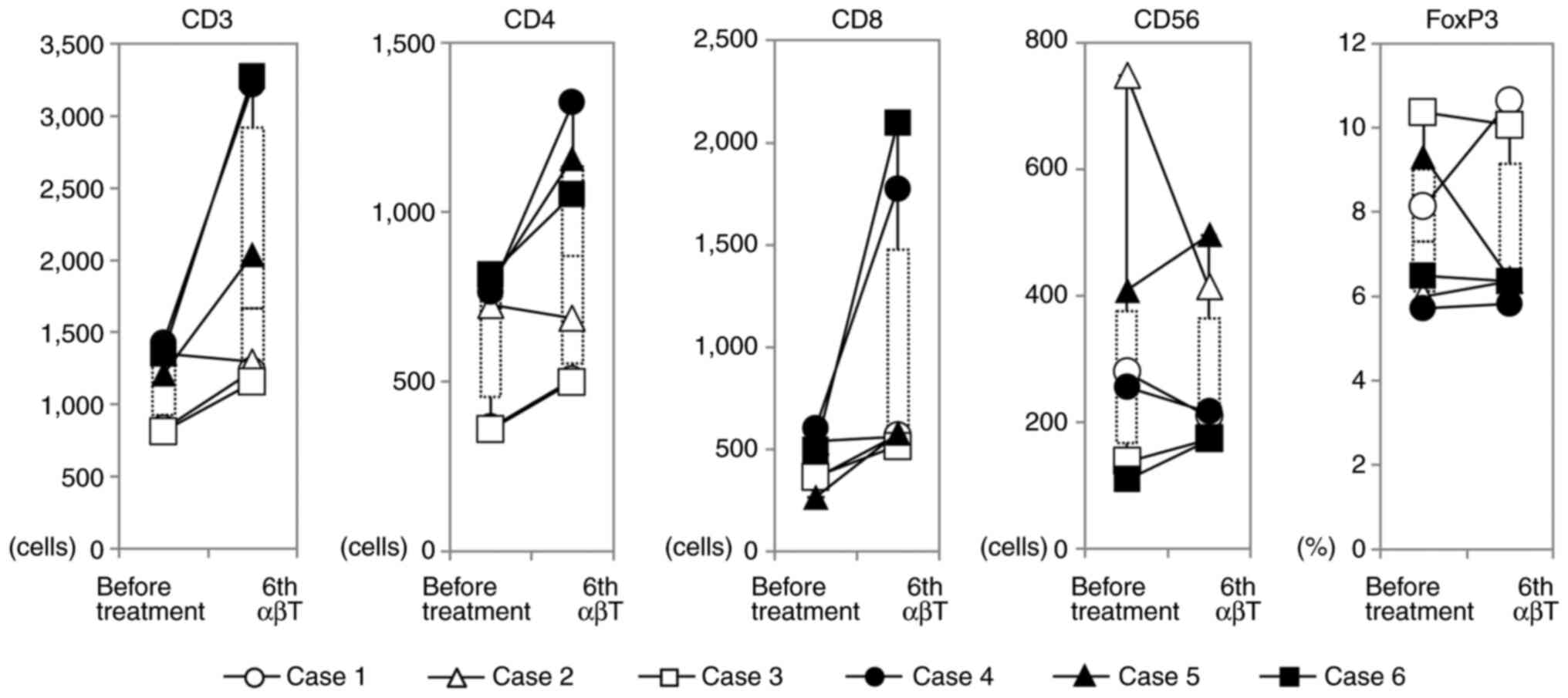
Changes in the number of immune cells, especially T lymphocytes, in peripheral blood before and after treatment were investigated using FCM. CD8+ T cells were markedly increased in cases 4 and 6 at the 6th administration of αβ T cells and slightly increased in the other four cases (P<0.01). After CAIT, CD8+ T cells were persistently increased in the peripheral blood in case 4, but CD8+ T cells promptly decreased in case 6 (Fig. 2). Analysis of CD4+ cells showed a significant increase in CD4+ T cells as well as CD8+ T cells in case 4, but in the other five cases, CD4+ T cells temporarily increased and returned to the pretreatment levels after treatment. In five cases, the number of CD56 positive NK cells did not change during treatment; however, in case 2, which showed the highest number of NK cells in peripheral blood before treatment, NK cells decreased by 50% after treatment (Fig. 3). In the patient with the highest peripheral blood γδ T cell ratio before treatment, Vγ9γδT cells increased after treatment and a transient increase in monocytes was observed, although the present treatment slightly reduced B cells in numerous cases (data not shown). There was no significant change in the regulatory T cell ratio in the peripheral blood (Fig. 3).
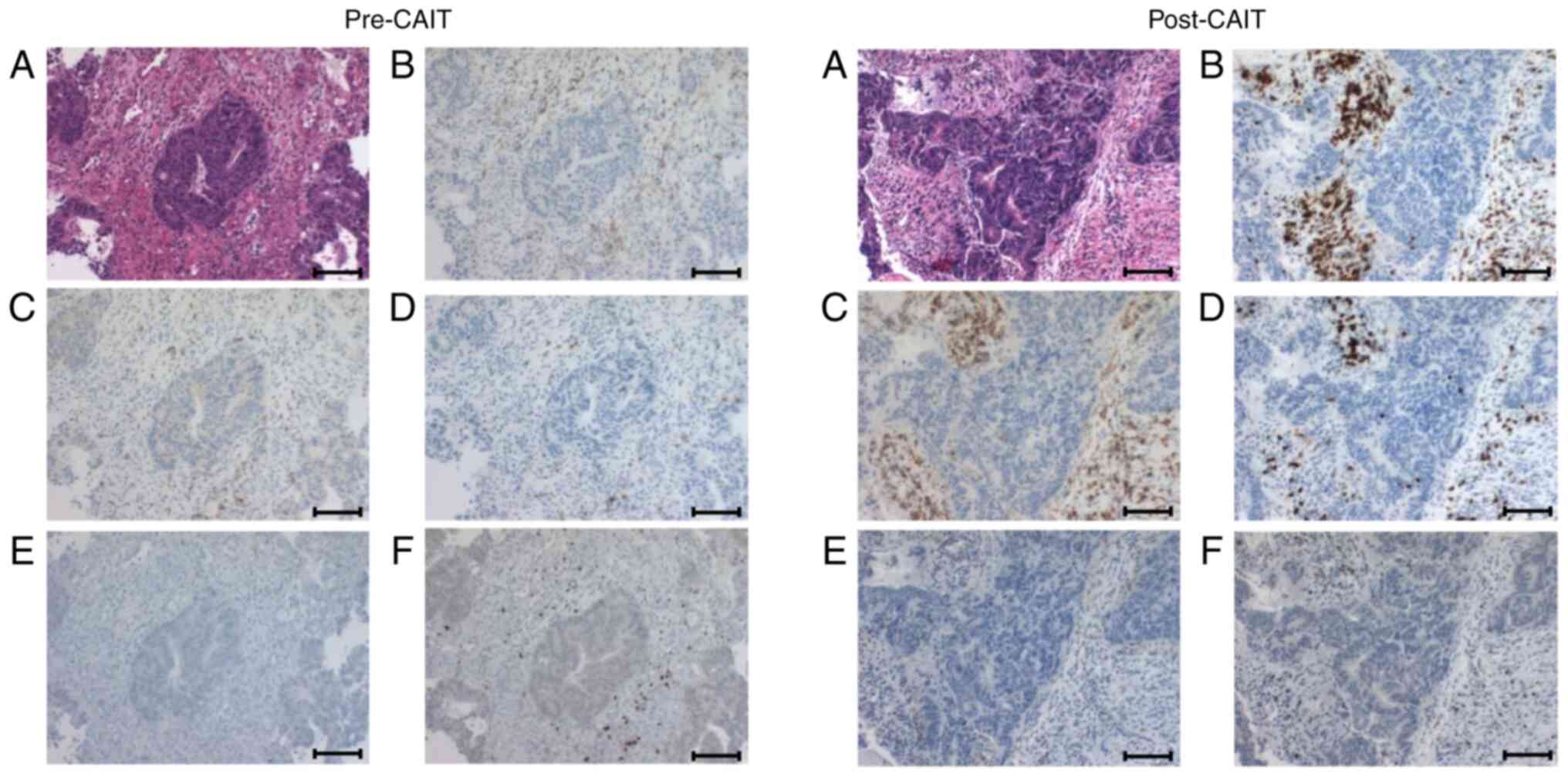
Immune cell infiltration changes in tumor tissues due to treatment were evaluated by immunohistochemical analysis (Fig. 4). In pretreatment biopsy tissue analysis, the proportion of tumor-infiltrating CD4+ T cells (range, 21.3–61.2%) was significantly higher than that of tumor-infilitrating CD8+ cells (range, 4.7–11.5%) in all cases. In two cases, CAIT enhanced CD8+ and reduced CD4+ T cell infiltration, respectively. Enhanced infiltration of both CD4+ and CD8+ T cells was observed in three cases. In case 6, infiltration of CD4+ T cells was higher than that of CD8+ T cells, although the infiltration of CD8+ T cells was reduced after treatment. The CD4+:CD8+ T cell ratio decreased after treatment in five cases (Table III).
Table III.CD4+ and CD8+ T cell infiltration changes due to treatment in tumor tissues were evaluated by immunohistochemical assays. |
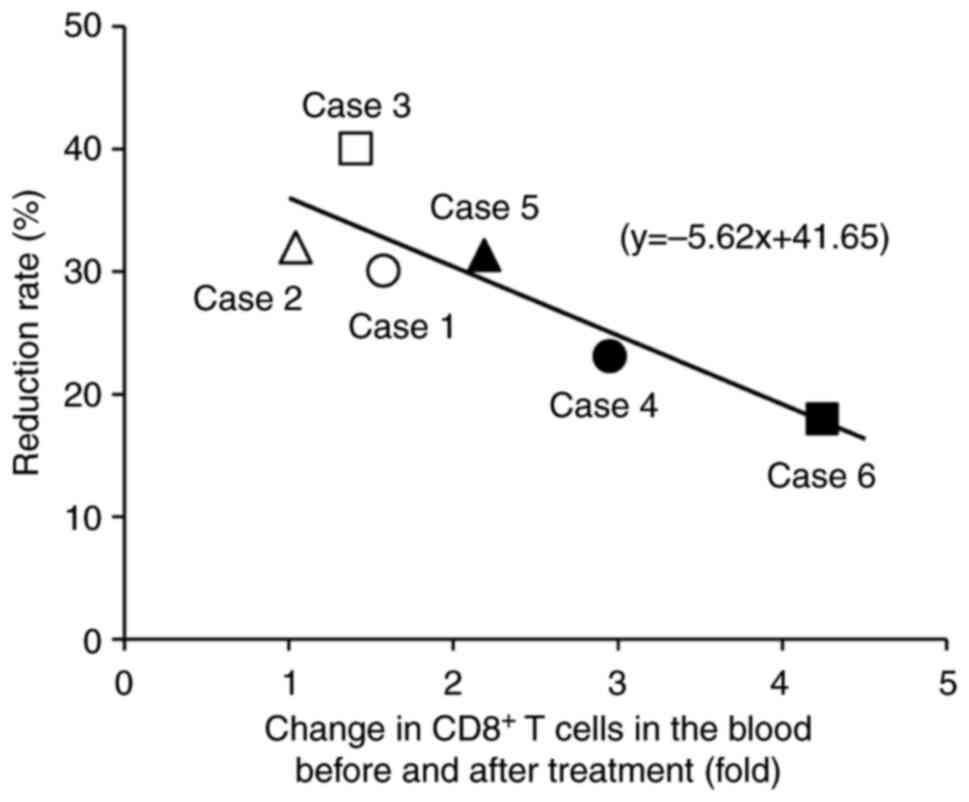
The relationship between antitumor effects, changes in T cells in the peripheral blood, and the degree of T cell infiltration were investigated in the tumor tissue. A single regression analysis showed a significant inverse correlation between antitumor response rates and the increased rate of peripheral blood CD8+ T cells after treatment (Fig. 5). Therefore, the smaller the increase in CD8+ T cells in the peripheral blood, the greater the reduction in tumor size. However, there was no notable relationship between changes in peripheral blood T cells and T cell infiltration into the tumor. Postoperative surveillance using CT and MRI will be scheduled for ≥5 years.
Discussion
A prospective, non-randomized, open-label, single-arm, translational clinical trial was conducted to evaluate the safety of neoadjuvant CAIT for advanced rectal cancer. The present study suggested that neoadjuvant CAIT can be safely administered for LARC.
In Europe and in the United States, NACRT + TME + adjuvant chemotherapy is the standard treatment for LARC (1). In Japan, TME with lateral lymph node dissection is the standard treatment. Since survival and LR-free rates in Japan have been reported to be higher than those in Europe and in the United States, the need for preoperative treatment has not been well established. However, even in Japan, the number of facilities that perform NACRT to control LR is increasing. Despite the positive surgical results in Japan, the option for NAC is routinely considered to avoid adverse events by radiotherapy and improve survival rate by controlling distant metastasis. Although there are few clinical trials on NAC in Japan, a multicenter phase II trial (FACT trial) verified the efficacy and safety of mFOLFOX6 therapy for stages II and III rectal cancer cases of cT3 and T4 (20–22). The study mentioned serious adverse events of grade 3–4 were neutropenia (9.6%), leukopenia (1.9%), thrombocytopenia (1.9%), febrile neutropenia (1.9%), nausea (1.9%), vomiting (1.9%) and peripheral neuropathy (3.8%) (22). The treatment completion rate was 80.8%, which was higher than that of postoperative adjuvant chemotherapy containing oxaliplatin in the MOSAIC trial (74.7%) (23) or the JOIN trial (67.0%) (24). In the current study, grade 3–4 neutropenia occurred in three patients (50%), thrombocytopenia in one patient (16.7%) and peripheral neuropathy in one patient (16.7%). The reason for the high adverse event rate was the small number of eligible patients. The treatment completion rate in the current study was 83.3%, which was similar with that of the FACT trial (84.5%). The median relative dose intensity was 100% for bolus fluorouracil and continuous infusion of fluorouracil, and 98% for oxaliplatin, which was higher than those in the FACT trial (93.2%). In addition, the disease control rate was 100%, and all patients underwent surgery with an R0 resection. These results were satisfactory compared with those of other trials (22–24). A meta-analysis of NAC and NACRT for advanced rectal cancer was reported in 2021 (25). No notable differences were found between the two groups regarding the pathological CR (pCR) rate, N downstaging rate, R0 resection rate, LR rate, and adverse events related to NAC and NACRT. Based on the current data, NAC could be considered as a reasonable alternative to NACRT in patients with T2/3 LARC. However, high-risk cases, such as T4b, have been reported to have a high LR rate (7.2%) and short OS (7.5 months) because NAC does not involve radiotherapy (5,25). The additional use of bevacizumab would contribute to a higher pCR rate and an improved response rate; however, a high suture failure rate (27.8%) was reported, which was thought to be caused by the addition of bevacizumab, the safety of which has not been established yet (20).
In the present study, changes in immune cells in the tumor microenvironment and peripheral blood were evaluated. After treatment, immunohistochemical analysis showed that CD8+ T cells increased in five cases in the tumor microenvironment. Analysis of the association between pCR rate and TIL in NAC has shown that the TIL level is a predictor of pCR being independent of other clinical pathological factors including tumor size, lymph node status and age, and chemotherapy including treatment with doxorubicin, cyclophosphamide and/or taxane regimens (26). In the current study, pCR in patients with rectal cancer receiving neoadjuvant CAIT was not obtained, although an increased rate of CD8+ T cells was found in the tumor after treatment. Moreover, high CD8+ TIL and a high CD8:Foxp3 ratio in residual tumors could predict improved prognosis in patients with triple-negative breast cancer without pCR following NAC (27). Therefore, it is necessary to carefully observe the prognosis of the present cases with non-pCR because, in most cases, CD8+ T cells and CD8:Foxp3 ratios were increased after NAC in the tumors. In colorectal cancer, patients with a low CD4+:CD8+ T cell ratio in tumors showed a notably higher 5-year survival rate and better prognosis than patients with a high CD4+:CD8+ T cell ratio, regardless of the stage or age (28). In five cases, a CD4+:CD8+ ratio reduction was observed, but in case 6, the number of CD8+ T cells decreased post neoadjuvant CAIT, while the CD4+:CD8+ ratio increased, and early recurrence was observed. For rectal cancer treated with neoadjuvant CAIT, these results indicated that the evaluation of immune cells, especially CD8+ T cells in the tumor microenvironment, could be useful as a biomarker for prognosis.
In most cases that received immune cell therapy, an increase in CD8+ T cell number in peripheral blood after treatment was previously reported (18). In patients treated with immune cell therapy combined with mFOLFOX6 as a preoperative therapy for rectal cancer, the increase in CD8+ T cells in the peripheral blood was notably lower than that in patients treated with immune cell therapy alone. In the present study, tumor infiltration of activated T cells was promoted by mFOLFOX6, and it was reported that FOLFOX treatment could induce an increase in the frequency and number of tumor-infiltrating CD8+ T cells in murine colon cancer models (29). Furthermore, there was a notable inverse association between the rate of increase in peripheral blood CD8+ T cells and the antitumor response rate. These results support the possibility that intratumoral infiltration of administered immune cells was promoted by combination with chemotherapy. Although neoantigen-specific T cells have the potential to cause high tumor regression (30), it has been observed that cancer-independent bystander CD8+ T cells are present in TILs for human colorectal and lung cancers, which recognize a wide range of epitopes unrelated to cancer (31). These bystander CD8+ T cells in the peripheral blood were expanded to induce antitumor immune activity in the present study.
To improve the pCR rate, it may be useful to use radiation therapy or ICIs in combination with concurrent immune cell therapy. NACRT, followed by ICI, has been reported to increase the pCR rate for rectal cancer. In microsatellite stability cases in which nivolumab, an ICI, was administered after chemoradiotherapy and before surgery, the pCR rate was 30% (32). In addition, the usefulness of immune cell therapy in combination with ICIs was reported for advanced and recurrent cancers (33).
The current study showed that neoadjuvant CAIT could be safely used for the treatment of advanced rectal cancer. However, the current study had several limitations. Due to the small sample size, statistical analysis was limited and could not provide definitive conclusions. Additionally, there was an imbalance between the number of male and female patients, which may have influenced the results. In the future, a large-cohort study of the comprehensive immunotherapy for LARC will be carried out to examine the effect of CAIT. It is crucial to study the effectiveness of comprehensive immunotherapy combining various treatments, such as chemoradiotherapy, surgery, ICI, and immune cell therapy, as the addition of immunotherapy to previously established treatments may potentially improve the effectiveness of cancer treatment. In addition, verifying the additional effect of CAIT compared with standard treatment is key.
Acknowledgements
Not applicable.
Funding
Funding: No funding was received.
Availability of data and materials
The datasets generated and/or analyzed during the current study are not publicly available due to privacy reasons but are available from the corresponding author on reasonable request.
Authors' contributions
YO, KSu, TI, AM, TaY, TeY, YY, SH and KSa acquired data. HI, SO, EO, SG, RT and TK carried out immunological analyzing and interpretation of data. TK and KSa drafted the original manuscript and guided the study. All authors read and approved the final manuscript. YO, TK and KSa confirm the authenticity of all the raw data.
Ethics approval and consent to participate
The present study was carried out in accordance with the Declaration of Helsinki. The current study was registered with the jRCT; ID, jRCTc030190248. The relevant Accreditation Committee for Regenerative Medicine (Tokyo, Japan) reviewed and approved this study. The IRBs of all participating institutions approved the present clinical study (Juntendo University, Tokyo, Japan; approval no. 2018061; Nippon Medical School, Tokyo, Japan; approval no. 2018-212), and written informed consent was obtained from every patient.
Patient consent for publication
All the patients enrolled in the present study agreed for their data to be published.
Competing interests
The authors declare that they have no competing interests.
References
|
Benson AB, Venook AP, Al Hawary MM, Cederquist L, Chen Y, Ciombor KK, Cohen S, Cooper HS, Deming D, Engstrom PF, et al: Rectal cancer, version 2.2018, NCCN clinical practice guidelines in oncology. J Natl Compr Canc Netw. 16:874–901. 2018. View Article : Google Scholar : PubMed/NCBI | |
|
Peeters KCMJ, Marijnen CAM, Nagtegaal ID, Kranenbarg EK, Putter H, Wiggers T, Rutten H, Pahlman L, Glimelius B, Leer JW, et al: The TME trial after a median follow-up of 6 years: Increased local control but no survival benefit in irradiated patients with resectable rectal carcinoma. Ann Surg. 246:693–701. 2007. View Article : Google Scholar : PubMed/NCBI | |
|
Folkesson J, Birgisson H, Pahlman L, Cedermark B, Glimelius B and Gunnarsson U: Swedish rectal cancer trial: Long lasting benefits from radiotherapy on survival and local recurrence rate. J Clin Oncol. 23:5644–5650. 2005. View Article : Google Scholar : PubMed/NCBI | |
|
Sauer R, Liersch T, Merkel S, Fietkau R, Hohenberger W, Hess C, Becker H, Raab HR, Villanueva MT, Witzigmann H, et al: Preoperative versus postoperative chemoradiotherapy for locally advanced rectal cancer: Results of the German CAO/ARO/AIO-94 randomized phase III trial after a median follow-up of 11 years. J Clin Oncol. 30:1926–1933. 2012. View Article : Google Scholar : PubMed/NCBI | |
|
Tomida A, Uehara K, Hiramatsu K, Maeda A, Sakamoto E, Okada Y, Kurumiya Y, Nakayama G, Nakamura M, Aiba T, et al: Neoadjuvant CAPOX and bevacizumab alone for locally advanced rectal cancer: Long-term results from the N-SOG 03 trial. Int J Clin Oncol. 24:403–410. 2019. View Article : Google Scholar : PubMed/NCBI | |
|
Benson AB, Venook AP, Al-Hawary MM, Arain MA, Chen YJ, Ciombor KK, Cohen S, Cooper HS, Deming D, Garrido-Laguna I, et al: NCCN guidelines insights: Rectal cancer, version 6.2020. J Natl Compr Canc Netw. 18:806–815. 2020. View Article : Google Scholar : PubMed/NCBI | |
|
Takayama T, Sekine T, Makuuchi M, Yamasaki S, Kosuge T, Yamamoto J, Shimada K, Sakamoto M, Hirohashi S, Ohashi Y and Kakizoe T: Adoptive immunotherapy to lower postsurgical recurrence rates of hepatocellular carcinoma: A randomised trial. Lancet. 356:802–807. 2000. View Article : Google Scholar : PubMed/NCBI | |
|
Iwai K, Soejima K, Kudoh S, Umezato Y, Kaneko T, Yoshimori K, Tokuda H, Yamaguchi T, Mizoo A, Setoguchi Y, et al: Extended survival observed in adoptive activated T lymphocyte immunotherapy for advanced lung cancer: Results of a multicenter historical cohort study. Cancer Immunol Immunother. 61:1781–1790. 2012. View Article : Google Scholar : PubMed/NCBI | |
|
Hodi FS, O'Day SJ, McDermott DF, Weber RW, Sosman JA, Haanen JB, Gonzalez R, Robert C, Schadendorf D, Hassel JC, et al: Improved survival with ipilimumab in patients with metastatic melanoma. N Engl J Med. 363:711–723. 2010. View Article : Google Scholar : PubMed/NCBI | |
|
Abbasi S, Totmaj MA, Abbasi M, Hajazimian S, Goleij P, Behroozi J, Shademan B, Isazadeh A and Baradaran B: Chimeric antigen receptor T (CAR-T) cells: Novel cell therapy for hematological malignancies. Cancer Med. 12:7844–7858. 2023. View Article : Google Scholar : PubMed/NCBI | |
|
Mulé JJ, Shu S, Schwarz SL and Rosenberg SA: Adoptive immunotherapy of established pulmonary metastases with LAK cells and recombinant interleukin-2. Science. 225:1487–1489. 1984. View Article : Google Scholar : PubMed/NCBI | |
|
Yoshida Y, Naito M, Yamada T, Aisu N, Daibo K, Mera T, Tanaka T, Naito K, Yasumoto K, Kamigaki T, et al: Adoptive chemoimmunotherapy using activated αβ T cells for stage IV colorectal cancer. Anticancer Res. 36:3741–3746. 2016.PubMed/NCBI | |
|
Brierley JD, Gospodarowicz MK and Wittekind C: TNM Classification of Malignant Tumours. 8th edition. John Wiley & Sons; Hoboken: 2017 | |
|
Oken MM, Creech RH, Tormey DC, Horton J, Davis TE, McFadden ET and Carbone PP: Toxicity and response criteria of the eastern cooperative oncology group. Am J Clin Oncol. 5:649–655. 1982. View Article : Google Scholar : PubMed/NCBI | |
|
National Cancer Institute, . Common Terminology Criteria for Adverse Events v4.0. August 24–2021https://ctep.cancer.gov/protocoldevelopment/electronic_applications/ctc.htm | |
|
Eisenhauer EA, Therasse P, Bogaerts J, Schwartz LH, Sargent D, Ford R, Dancey J, Arbuck S, Gwyther S, Mooney M, et al: New response evaluation criteria in solid tumours: Revised RECIST guideline (version 1.1). Eur J Cancer. 45:228–247. 2009. View Article : Google Scholar : PubMed/NCBI | |
|
Japanese Society for Cancer of the Colon Rectum, . Japanese classification of colorectal, appendiceal, and anal carcinoma: The 3-d, english edition [Secondary Publication]. J Anus Rectum Colon. 3:175–195. 2019. View Article : Google Scholar : PubMed/NCBI | |
|
Kamigaki T, Ibe H, Okada S, Matsuda E, Tanaka M, Oguma E, Kinoshita Y, Ogasawara S, Ono A, Makita K, et al: Improvement of impaired immunological status of patients with various types of advanced cancers by autologous immune cell therapy. Anticancer Res. 35:4535–4543. 2015.PubMed/NCBI | |
|
Ishii F, Yoshida Y, Yamauchi Y, Aisu N, Kojima D, Mera T, Kato D, Tanaka T, Naito K, Yasumoto K, et al: Hepatectomy for liver metastases of colorectal cancer after adoptive chemoimmunotherapy using activated αβ T-cells. Anticancer Res. 37:3933–3939. 2017.PubMed/NCBI | |
|
Uehara K, Hiramatsu K, Maeda A, Sakamoto E, Inoue M, Kobayashi S, Tojima Y, Yoshioka Y, Nakayama G, Yatsuya H, et al: Neoadjuvant oxaliplatin and capecitabine and bevacizumab without radiotherapy for poor-risk rectal cancer: N-SOG 03 phase II trial. Jpn J Clin Oncol. 43:964–971. 2013. View Article : Google Scholar : PubMed/NCBI | |
|
Kamiya T, Uehara K, Nakayama G, Ishigure K, Kobayashi S, Hiramatsu K, Nakayama H, Yamashita K, Sakamoto E, Tojima Y, et al: Early results of multicenter phase II trial of perioperative oxaliplatin and capecitabine without radiotherapy for high-risk rectal cancer: CORONA I study. Eur J Surg Oncol. 42:829–835. 2016. View Article : Google Scholar : PubMed/NCBI | |
|
Hasegawa H, Okabayashi K, Tsuruta M, Koike J, Funahashi K, Yokomizo H, Yoshimatsu H, Kan H, Yamada T, Ishida H, et al: Updated survival results of FACT trial: Multicenter phase II trial of neoadjuvant chemotherapy with mFOLFOX6 for stage II/III rectal cancer with a T3/T4 tumor. Ann Oncol. 28:v171–v172. 2017. View Article : Google Scholar | |
|
André T, Boni C, Navarro M, Tabernero J, Hickish T, Topham C, Bonetti A, Clingan P, Bridgewater J, Rivera F and de Gramont A: Improved overall survival with oxaliplatin, fluorouracil, and leucovorin as adjuvant treatment in stage II or III colon cancer in the MOSAIC trial. J Clin Oncol. 27:3109–3116. 2009. View Article : Google Scholar : PubMed/NCBI | |
|
Kotaka M, Yoshino T, Oba K, Shinozaki K, Touyama T, Manaka D, Matsui T, Ishigure K, Hasegawa J, Inoue K, et al: Initial safety report on the tolerability of modified FOLFOX6 as adjuvant therapy in patients with curatively resected stage II or III colon cancer (JFMC41-1001-C2: JOIN trial). Cancer Chemother Pharmacol. 76:75–84. 2015. View Article : Google Scholar : PubMed/NCBI | |
|
Lin H, Wang L, Zhong X, Zhang X, Shao L and Wu J: Meta-analysis of neoadjuvant chemotherapy versus neoadjuvant chemoradiotherapy for locally advanced rectal cancer. World J Surg Oncol. 19:1412021. View Article : Google Scholar : PubMed/NCBI | |
|
Adams S, Gray RJ, Demaria S, Goldstein L, Perez EA, Shulman LN, Martino S, Wang M, Jones VE, Saphner TJ, et al: Prognostic value of tumor-infiltrating lymphocytes in triple-negative breast cancers from two phase III randomized adjuvant breast cancer trials: ECOG 2197 and ECOG 1199. J Clin Oncol. 32:2959–2966. 2014. View Article : Google Scholar : PubMed/NCBI | |
|
Miyashita M, Sasano H, Tamaki K, Hirakawa H, Takahashi Y, Nakagawa S, Watanabe G, Tada H, Suzuki A, Ohuchi N and Ishida T: Prognostic significance of tumor-infiltrating CD8+ and FOXP3+ lymphocytes in residual tumors and alterations in these parameters after neoadjuvant chemotherapy in triple-negative breast cancer: A retrospective multicenter study. Breast Cancer Res. 17:1242015. View Article : Google Scholar : PubMed/NCBI | |
|
Diederichsen AC, Hjelmborg Jv, Christensen PB, Zeuthen J and Fenger C: Prognostic value of the CD4+/CD8+ ratio of tumour infiltrating lymphocytes in colorectal cancer and HLA-DR expression on tumour cells. Cancer Immunol Immunother. 52:423–428. 2003. View Article : Google Scholar : PubMed/NCBI | |
|
Mosely SI, Prime JE, Sainson RC, Koopmann JO, Wang DY, Greenawalt DM, Ahdesmaki MJ, Leyland R, Mullins S, Pacelli L, et al: Rational selection of syngeneic preclinical tumor models for immunotherapeutic drug discovery. Cancer Immunol Res. 5:29–41. 2017. View Article : Google Scholar : PubMed/NCBI | |
|
Li Q and Ding ZY: The ways of isolating neoantigen-specific T cells. Front Oncol. 10:13472020. View Article : Google Scholar : PubMed/NCBI | |
|
Simoni Y, Becht E, Fehlings M, Loh CY, Koo SL, Teng KWW, Yeong JPS, Nahar R, Zhang T, Kared H, et al: Bystander CD8+ T cells are abundant and phenotypically distinct in human tumour infiltrates. Nature. 557:575–579. 2018. View Article : Google Scholar : PubMed/NCBI | |
|
Bando H, Tsukada Y, Inamori K, Togashi Y, Koyama S, Kotani D, Fukuoka S, Yuki S, Komatsu Y, Homma S, et al: Preoperative chemoradiotherapy plus nivolumab before surgery in patients with microsatellite stable and microsatellite instability-high locally advanced rectal cancer. Clin Cancer Res. 28:1136–1146. 2022. View Article : Google Scholar : PubMed/NCBI | |
|
Takimoto R, Kamigaki T, Gotoda T, Takahashi T, Okada S, Ibe H, Oguma E and Goto S: Esophageal cancer responsive to the combination of immune cell therapy and low-dose nivolumab: Two case reports. J Med Case Rep. 15:1912021. View Article : Google Scholar : PubMed/NCBI |